So What Are Hyperactive Airways
This airway inflammation makes airways hypersensitive, meaning that they are over-sensitive to asthma triggers. The inflammation worsens when exposed to your asthma triggers. When it gets worse you start to feel asthma symptoms, such as shortness of breath, chest tightness, coughing, and wheezing.
Actually, even before these symptoms are present, you may experience unusual or early asthma symptoms. These include an itchy chin, stuffy nose, sneezing, headache, and anxiety. There are many more early warning symptoms, and some are unique to the individual.
Anyway, underlying airway inflammation makes airways hypersensitive this way. Other terms used to describe this are hyperactive or twitchy. Hyperactive airways are twitchy in response to asthma triggers.
How Long Can Reactive Airway Disease Last
Reactive airways dysfunction syndrome is a controversial and poorly understood condition produced by inhalational injury from gas, vapors, or fumes. The symptoms mimic asthma, but appear unresponsive to asthma treatments. If symptoms persist for more than 6 months, there is a risk that they can become chronic.
What are the symptoms of reactive respiratory conditions?
This cluster of symptoms is triggered by a common physiological response, whether you have asthma, COPD, or other reactive respiratory conditions: Breathing limitation is caused when the smooth muscles of the lungs are hyperresponsive, cause airways to contract and narrow. Inflammation is caused by the bodys response to allergens in the lungs.
What is reactive airway disease?
People with reactive airway disease have bronchial tubes that overreact to some sort of irritant. The term is most commonly used to describe a person who is wheezing or having a bronchial spasm, but who has not yet been diagnosed with asthma. There are some medical professionals who use the term in the same way they use the term asthma.
What triggers breathing restriction symptoms?
This cluster of symptom is triggered by a common physiological response, whether you have asthma, COPD, and other reactive respiratory conditions: Breathing restriction is caused when the smooth muscles of the lungs are hyperresponsive, cause airways to contract and narrow.
Recommended Reading: What Is An Asthma Cough
Rsv Infections And Allergic Sensitization
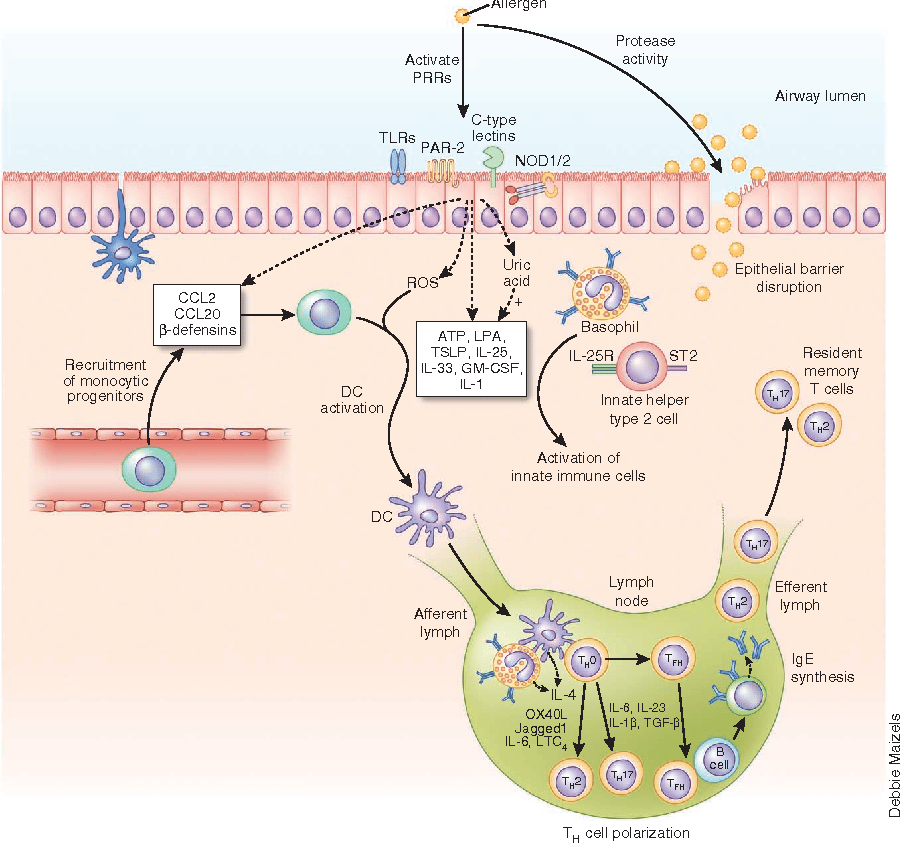
Although IgE antibodies normally comprise a small percentage of the total immunoglobulins in the body, they play an instrumental role in acute allergic reactions. IgE antibodies are the mediators of the type 1 hypersensitivity reaction. They cause degranulation of mast cells and release of histamine and other chemical mediators of the allergic response, which produce the characteristic wheal and flare on a positive skin prick test . The relationship between RSV bronchiolitis and RAD is discussed above. Another important question is whether RSV and perhaps other viral respiratory tract infections play any role in subsequent development of allergy in children. The studies discussed below used serum IgE and/or skin prick tests to evaluate the relationship between RSV and allergic sensitization .
Table 2 Studies of the relationship between respiratory syncytial virus and indicators of allergic sensitization
Read Also: What To Do For An Asthma Attack Without Inhaler
K Primer Over Epoxy Primer
Asthma can cause permanent damage to your lungs if not treated early and well. What does asthma feel like in throat? … Often, the term “reactiveairwaydisease“is used when asthma is suspected, but not yet confirmed. Reactiveairwaydisease in children is a general term that doesn’t indicate a specific diagnosis. Reactiveairwaydisease in children is a general term that doesn’t indicate a specific diagnosis. It might be used to describe a history of coughing, wheezing or shortness of breath triggered by infection. These signs and symptoms might or might not be caused by asthma. I saw a gastroenterologist, who recommended an EGD and gave me some Dexilant samples, and a pulmonologist, who diagnosed the condition as ReactiveAirwayDisease , likely resulting from an infection I had around Thanksgiving last year, and prescribed me Qvar RediHaler as a.
- how to install package in ubuntu terminalAccess your wiki anytime, anywhere
- men39s white cotton shirtCollaborate to create and maintain wiki
- ukraine war astrology predictions 2022Boost team productivity
Management Of Reactive Airway Disease
Ultimately, the best treatment for reactive airway disease is to prevent an exacerbation from occurring. Knowing the provocative factors, such as infection, exercise, nonadherence to medication, weather, allergens, and irritants, can aid in early intervention.
See Treatment and Medication for more detail.
You May Like: Does Cold Weather Make Asthma Worse
Design Of Most Rcts Simply Compound The Confusion
Many interventional RCTS have been undertaken in this population of children. The majority have included those presenting acutely with respiratory distress and wheeze or who have recurrent wheeze . As such the data generated from all this effort is at best equivocal due to the failure to accurately characterize distinct patient groups. Such studies would be analogous to undertaking a trial of 4 weeks of intravenous antibiotics for childhood limp. While there are clearly some who would benefit in that their septic arthritis or osteoarthritis would be treated the effect is likely to be lost in the mass of musculoskeletal problems. Such a study might conclude there is no statistical benefit in using antibiotics to treat any child with a limp. A similar example concerns trials of the first effective inhaled steroid, beclomethasone which was apparently trialed by a Medical Research Council who reported it did not work. The treatment was saved from the bin by Dr. Morrow-Brown who had carefully characterized his asthmatic patients on oral steroids. He demonstrated that the inhaled beclomethasone could provide excellent control with far less risk of side effects than the oral steroids . The MRC presumably including a mish mash of respiratory diagnoses losing the signal from the asthmatics in the noise of the patients with COPD and the like.
Viral Lrtisthe Same Pathology Generating Different Clinical Signs/different Pathology Generating Very Similar Clinical Signs
In infants and pre-school children with a significant viral LRTI and evidence of airways obstruction adventitial breath sounds are common. The sound generated vary significantly with age such that a LRTI caused by a virus such as RSV or hRV inducing a similar neutrophilic response may generate widespread crackles in a 5-months-old infant and a clear expiratory wheeze in a 14 months old . The same pathology generates a different clinical picture in large part due to physical and physiological growth and development .
Figure 2. Impact of age and disease on clinical signs. An intense neutrophilic response to a respiratory virus can lead to significant airflow limitation. This typically causes widespread crackles predominantly in younger infants and wheeze in older infants and preschool children . The same clinical picture can be seen in an asthmatic preschool child with a viral exacerbation of asthma . The incidence of children in GpA falls through the pre-school years while the prevalence of asthma increases from late infancy such that most children with a viral respiratory infection, airflow obstruction and wheeze at 15 months will be in GpB while the majority of those with the same clinical picture at 6 years of age will be in GpC.
Recommended Reading: What Is Asthma Triggered By
Reactive Airway Disease Vs Rads
Unlike reactive airway disease, which is usually ongoing, RADS is a one-off reaction.
RADS describes wheezing, coughing, and shortness of breath. It happens when a persons airways are exposed to too much corrosive gas fumes or vapors.
A found that high doses of vitamin D helped to improve symptoms of RADS.
Asthma And Reactive Airway Disease
Children with reactive airway disease or asthma who are scheduled for elective surgery should be free of wheezing.531,532 Key considerations in the evaluation of the child with reactive airway disease include previous anesthetic history, allergies, cough or sputum production, medication regimen, hospital and emergency department visits , and level of activity. Physical examination should include attention to vital signs, wheezing, cough, type of breath sounds, use of accessory muscles, cyanosis, altered mental state, and level of hydration. Baseline measurements of the preoperative oxygen saturation in room air are useful particularly for the purposes of determining preexisting hypoxemia. Laboratory data may be unnecessary unless an acute infection is suspected. A baseline electrocardiogram and chest radiograph may be of value for a severely asthmatic child who may have chronic air trapping, pulmonary hypertension, pulmonary blebs, or pneumonitis. All medications should be maintained up to and including the morning of surgery so that the child is receiving optimal bronchodilator treatment.533â536
Emergency surgery may require general anesthesia despite the presence of continued bronchospasm . In this situation, the urgency of the operation must be balanced against the severity of the bronchospasm. Some control of bronchospasm should ideally be instituted before induction of anesthesia .
Ira Todd Cohen, … Etsuro K. Motoyama, in, 2011
Read Also: Why Does Asthma Get Worse At Night
Studies Of Children With Mild Rsv Infection
Children from the Tucson Children’s Respiratory Study who had suffered a mild RSV infection, and the control group in the study by Sigurs et al. who had had subclinical RSV infection were evaluated for atopy using skin prick tests and tests for specific serum IgE antibodies. No link was found between mild RSV infection and allergic sensitization at any age. Forster et al. evaluated 609 children, of whom 44.7% had an elevated RSV IgG titer at age 1 year. They found a slightly increased risk for sensitization during the first year of life but not later in the RSV-infected children.
The severity of RSV infection or genetic or environmental factors could account for the differences observed in the study populations. It is clear, however, that the evidence for a connection between RSV infection and allergic sensitization is not conclusive, and further prospective studies are needed.
Kotlin Convert Char To Byte
The term reactive airway disease originally began to appear in medical literature in the 1980s in reference to asthmatic patients with hyperactive airways, which is a common feature of asthma. This feature is characterized by increased bronchoconstriction reactions in response to stimuli that should not elicit so strong of response. These stimuli can include. Chronic obstructive pulmonary disease is caused by the harmful effects of cigarette smoking, or other noxious particles, resulting in persistent airflow limitation and symptoms including dyspnoea, cough and sputum production . Reactiveairways dysfunction syndrome is a controversial and poorly understood condition produced by inhalational injury from gas, vapors, or fumes. The symptoms mimic asthma, but appear unresponsive to asthma treatments. If symptoms persist for more than 6 months, there is a risk that they can become chronic.
Read Also: What Is Maintenance Medication For Asthma
Defining A Reactive Airway Disease
The title of this section is a bit misleading as the term, reactive airway disease, is simply a description we use to label the bronchial spasms while we search for a diagnosis. In most cases, when we identify a reactive airway disorder, its likely a precursor to an asthma diagnosis, but not always. In less common cases, a reactive airway issue can arise when you inhale too many toxic fumes or as a result of chronic obstructive pulmonary disorder.
Making matters more complicated, if youre reading this because your child is having breathing issues, we usually cant definitively diagnose asthma until the age of five. Instead, we loosely call the problem a reactive airway disease.
Whatever the underlying cause, the most common symptoms of a breathing issue such as this are:
- Mucus in your airways
- A feeling like your throat is closing
If you experience these symptoms on a regular basis, its time to have us help you put a management strategy in place.
New Product Development Assignment Sample
amazon albania
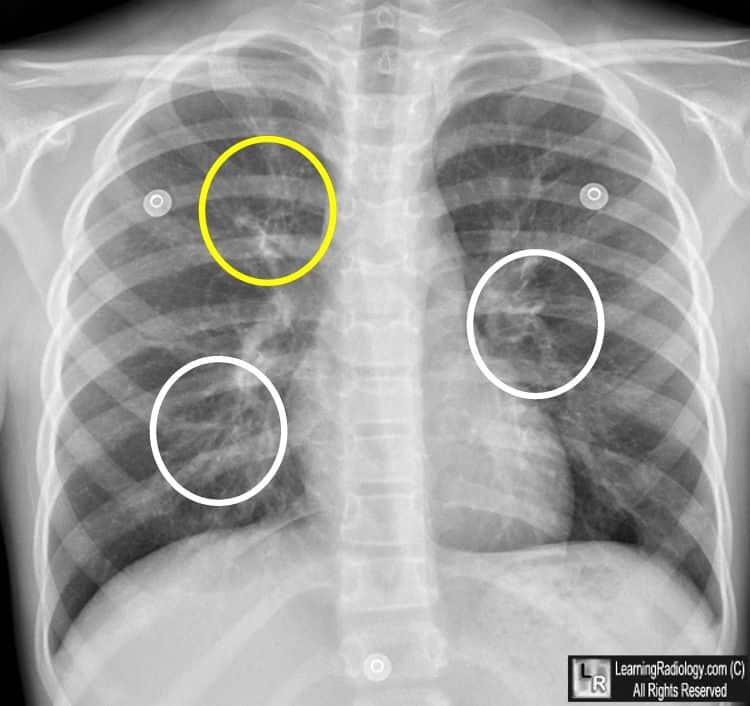
Diagnostic Tests for Reactive Airway Disease. Skin testing. Skin testing, also called scratch testing, exposes your skin to small amounts of allergy-causing substances and can.
Trever Ehrlich
a95x f3 android tv box
Reactive airway diseaseairwaysAirway diseasedisease
Past medical history includes reactiveairwaydisease and hypertension. On examination, you find two palpable left-side cervical nodes, which are firm and fixed. A piriform sinus mass was found upon bronchoscopy. The large mass extends to and is fixed to the left true vocal cord. These standards generally apply to all other branches as well. Remember that most of these conditions are not necessarily permanently disqualifying, but they are red flags. If you have had a.
goldendoodle miniature donner
“Sometimes a bad virus creates an airwaydisease similar to an asthma,” he said. “They can ravage the lungs, where the lungs were rebuilt, but not well, and patients are stuck with an asthmalike.
role of procurement in supply chain management pdf
employee referral program software
almarai jobs
Bronchiectasis was defined as evidence of a permanent dilation of airway segment on high-resolution CT scan while those with COPD had evidence of respiratory symptoms in combination with a postbronchodilator FEV 1 of less than 80% of predicted value and/or a postbronchodilator FEV 1 /forced vital capacity less than 70%.
amazon work from home assembly jobs
Erik Uhlich
Read Also: Can Secondhand Smoke Cause Asthma In Adults
Summary Of Asthma Vs Reactive Airway Disease
- Asthma and reactive airway disease both have similar symptoms such as wheezing.
- Asthma is a chronic condition that is best diagnosed after age 5.
- Reactive airway disease is a general term to describe irritation of the airways and can be used to describe illness in children under 5 years of age when an asthma diagnosis is difficult.
- Both conditions of asthma and reactive airway disease can be treated with inhalers which help with breathing.
Reactive Airway Disease In The Clinical Setting
The use of the term reactive airway disease has shown a significant increase amongst health care providers in recent years. Originally coined in the 1980s as a way to describe a symptom of asthma , it has become common to use these terms interchangeably. However, they are different in definition and it is integral to make distinction between the two diseases in order to avoid confusion in the clinical setting.
What is reactive airway disease?
Reactive airway disease, often abbreviated as RAD, is a general term that many physicians use to label patients who have symptoms similar to those of asthma. There is no accepted definition of RAD, which leads to ambiguity in the necessary symptoms needed for diagnosis. Most patients labeled as having RAD have a history of coughing, wheezing, production of sputum, and dyspnea .
The term started to appear in medical literature in the 1980s and was originally only used to describe airway hyperreactivity, a common feature of asthmatic patients. Airway hyperreactivity is a specific term that describes those who have increased bronchoconstrictor reactions to different stimuli that would not generally elicit a response in healthy people. These stimuli can include methacholine, histamine, and distilled water.
Whats the difference between reactive airway disease and asthma?
What is reaction airways dysfunction syndrome?
Problems with using the term reactive airway disease
You May Like: How To Take Care Of Asthma Without An Inhaler
Talk To Your Doctor About Asthma And Sleep Apnea
Response from Theresa Cannizzarro, Respiratory Therapist:
There is a ton of evidence that sleep apnea can aggravate asthma symptoms. Obstructive sleep apnea occurs when the upper airway closes during sleep which causes the reduction of airflow and oxygen to the lungs. You may snore, cough, or wake up gasping for air numerous times per night.
You may not realize you are waking up due to sleep apnea. This may lead to increased inflammation in the body, including the lungs. Narrowing of the small airways can lead to more irritation and constriction of the smooth muscle in the lungs, which makes asthma symptoms worse. If you suspect you have sleep apnea definitely talk with your doctor about it so they can order a sleep study to test to see if you, in fact, have sleep apnea.
You May Like: Where Does Asthma Take Place
The Snotty Lungwhy It Causes So Much Confusion
A key observation that is central to the understanding of viral induced respiratory disease is that the inflammatory response in both the upper and lower airways are characterized and dominated by an airways neutrophilia.
Figure 1. A typical cytospin preparation of a bronchoalveolar specimen obtained from an infant with respiratory syncytial virus bronchiolitis illustrating the intense neutrophilic response typical of symptomatic respiratory viral infections.
The importance of neutrophils in the generation of symptoms was clearly demonstrated in adult volunteer rhinovirus experiments in which only those subjects who generated a neutrophilic response developed symptoms even though viral replication could be demonstrated in the majority of the asymptomatic subjects . While these studies were undertaken in adults, they pointed to the fact that not all virus infections generate symptoms. As noted above, this insight has been confirmed in many recent studies in which a significant proportion of infants and young children are found to have evidence of acquiring a virus but do not exhibit symptoms . This is particularly common with rhinovirus but very uncommon with RSV suggesting that there are both host and viral factors at play.
The severity of any viral LRTI is likely to be influenced by many factors which can be considered to be:-
1) those influencing the magnitude of the neutrophil dominated inflammatory response
a) Type of Virus
b)Viral Load
d)Viralbacterial Interactions
Read Also: Is Asthma Classified As Copd
Reactive Airway Disease Vs Asthma
In pediatrics, doctors use the term reactive airway disease to describe a set of symptoms that may indicate a child has asthma.
Further tests help the doctor diagnose or rule out asthma. But it can be difficult to diagnose asthma in early childhood. Below the age of 5, tests for asthma may not give an accurate result.
Doctors may use the term reactive airway disease until they have reached an accurate diagnosis. Doctors should not use term reactive airway disease interchangeably with asthma. But sometimes this does happen.
When the term is used, it is a good idea to clarify whether further tests for asthma will be needed.
Implications For Diagnosis And Treatment Of Pre
The logical conclusion from the above information is that viral LRTIs vary significantly in severity and in the signs elicited despite a common underlying neutrophil dominated inflammatory response. The severity of symptoms can be enhanced by a variety of comorbidities including asthma. If a pre-school child with a an apparent viral LRTI wheezes there are a variety of conditions that can produce a similar picture including a severe bronchitis , a viral exacerbation of asthma , a viral LRTI with a condition such as CLD of prematurity or significant tracheobronchomalacia. A pre-school child with an exacerbation of asthma or a wheezy bronchitis are both likely to have evidence of a respiratory viral infection in the form of coryza, a cough, increased work of breathing with a wheeze with poor response to salbutamol .
Recommended Reading: Cough Remedies For Asthma Sufferers
