Will I Have To Take Medicine All The Time
Maybe not. Asthma is a chronic condition that is controllable. Unfortunately, there is no cure for asthma. For that reason, you may have asthma symptoms when exposed to triggers. This is the case even if you dont have symptoms very often. Your triggers can change over time, and your treatment will depend on two things: how severe your asthma is, and how often you have symptoms. If your asthma is controlled, your treatment will focus on managing symptoms and treatment of episodes when they happen.
If your symptoms happen at certain times and you know what caused them, you and your doctor can use this information to determine the best treatment. If, for example, you have seasonal asthma because of a specific pollen allergy, you may take medicines only when that pollen is in the air. But asthma that specific is not common. Many people with asthma take some form of medicine most or all of the time.
How Do You Use A Nebulizer
A nebulizer consists of the nebulizer machine, tubing, medicine cup, and mouthpiece or mask. The NIHs National Asthma Education and Prevention Program encourages people to follow the manufacturers instructions.
However, the offer the following steps to set up and use a nebulizer:
Will Medicine Help Me Sleep Better
Yes, if you have nighttime asthma symptoms. Many people wake up with asthma symptoms such as coughing or wheezing. You can control nighttime symptoms by taking asthma medicines as directed by your doctor.
Removing triggers where you sleep may help you sleep better. Many people are allergic to dust mites and mold found in bedding materials. Using mattress or pillow encasements can help contain those allergens. Dehumidifiers can also be helpful to reduce the humidity in your home that dust mites and mold need to exist. Using air cleaners in your bedroom may also help reduce your exposure to allergens and irritants .
Also Check: What’s An Asthma Attack Feel Like
How To Help Someone With An Asthma Attack Without An Inhaler
Asthma is a very common condition with around one in 13 of us affected. Its been increasing since the 1980s and affects people of all ages and backgrounds. Theres currently no cure for asthma, but typically with the right treatment plan and lifestyle changes, most people diagnosed with asthma are able to live normally without severe symptoms.
However, very occasionally, a person with asthma may be caught off guard. They might find themselves facing an attack without an inhaler to help them. Fortunately, this doesnt need to be as bad as it might sound. With the right assistance, they could get through an attack using some simple coping techniques.
If you know someone with asthma, learning more about their condition, as well as what you can do to help them, can be valuable.
Where Do You Get A Reliever Inhaler

You get a reliever inhaler from your GP or asthma nurse. Anyone with asthma, or suspected asthma, should be prescribed a reliever inhaler.
Make sure you contact your GP for a new prescription before your reliever inhaler runs out.
Some inhaler devices have a counter to show how many doses are left. When the numbers on the counter turn red, its time to contact your GP for a new prescription.
You can arrange repeat prescriptions with your local pharmacy to make things easier.
If for some reason you cant get a new prescription from the GP and you urgently need a replacement reliever inhaler, ask your pharmacist. They may be able to issue an emergency reliever.
Read Also: Ways To Relieve Asthma Without An Inhaler
What Other Information Should I Know
Keep all appointments with your doctor.
Do not let anyone else use your medication. Ask your pharmacist any questions you have about refilling your prescription.
It is important for you to keep a written list of all of the prescription and nonprescription medicines you are taking, as well as any products such as vitamins, minerals, or other dietary supplements. You should bring this list with you each time you visit a doctor or if you are admitted to a hospital. It is also important information to carry with you in case of emergencies.
How To Use A Metered Dose Inhaler
Inhalers are different, so check your instructions.
- Prime the inhaler first. You need to do this when you use an inhaler for the first time, or if you havenât used it for 2 weeks or more.
- Shake it for 5 seconds, turn the inhaler away from you, and press down to spray it.
- Wait a few seconds and do it again.
- Then do this two more times for a total of four.
Recommended Reading: Does Ibuprofen Make Asthma Worse
Watch How To Help Someone Who Is Having An Asthma Attack
What is asthma?
Asthma is a medical condition that affects the airways the tubes that carry air in and out of the lungs. When someone has an asthma attack, these tubes become narrowed, making it difficult to breathe in and out.
How can I tell if someone is having an asthma attack?
People with asthma should be able to let you know if they are having an attack.
Someone having an asthma attack will have difficulty breathing and speaking, and may cough and wheeze. They may be very anxious and distressed as they struggle to breathe.In some cases, their lips, earlobes and nail beds may turn greyish-blue because there isnt enough oxygen in their body.
What sort of medication will someone with asthma use?
Someone who has asthma will normally have an inhaler that their doctor has prescribed. They may also have a spacer, which makes the inhaler more effective.
If someone is having an asthma attack they should know how to use their inhaler and spacer but they may need your help in finding them.
What does an inhaler look like?
Inhalers can come in many different sizes and shapes. Inhalers to relieve asthma attacks are usually blue. Inhalers that prevent asthma attacks may be brown or white.
How do you use an inhaler?
If a person has asthma they should know how to use their inhaler, they may need your help getting it for them. They should take it as normal. If that doesnt help they can take one or two puffs every 30 or 60 seconds until theyve had 10 puffs.
Do People With Asthma Face A Higher Risk Of Severe Illness If They Get Covid
Theres a lot we still dont know about COVID-19 and how it affects asthma patients.
Based on the data we have so far, asthma does not appear to increase the risk of acquiring COVID-19. However, the Centers for Disease Control and Prevention does list chronic lung disease or moderate to severe asthma under groups at higher risk for severe illness if they get COVID-19.
Its important to understand what severe illness means.
One complication from COVID-19 is acute respiratory distress syndrome, a severe lung disease that results from damage to the alveoli, the air sacs of the lungs. When COVID-19 patients require ventilators, its often for acute respiratory distress syndrome. We dont know very much about the risk factors for developing acute respiratory distress syndrome or how to treat the specific type of inflammation that drives this condition, but there is no evidence that asthma is a risk factor for developing acute respiratory distress syndrome if infected with COVID-19.
In contrast to acute respiratory distress syndrome, asthma is a chronic condition that we know a lot about. It is characterized by airway inflammation, mucous production and airway spasm. Respiratory viruses, including strains of coronavirus that cause the common cold, can trigger asthma symptoms, and its likely that COVID-19 could do the same. Even though asthma is also an inflammatory condition, in contrast to acute respiratory distress syndrome, we have very effective treatments for asthma.
Also Check: Long Term Use Of Albuterol Inhalers
What Are Common Asthma Attack Triggers
An asthma attack happens when someone comes in contact with substances that irritate them. Healthcare providers call these substances triggers. Knowing what triggers your asthma makes it easier to avoid asthma attacks.
For some people, a trigger can bring on an attack right away. Sometimes, an attack may start hours or days later.
Triggers can be different for each person. But some common triggers include:
- Air pollution: Many things outside can cause an asthma attack. Air pollution includes factory emissions, car exhaust, wildfire smoke and more.
- Dust mites: You cant see these bugs, but they are in many homes. If you have a dust mite allergy, they can cause an asthma attack.
- Exercise: For some people, exercising can cause an attack.
- Mold: Damp places can spawn mold. It can cause problems for people with asthma. You dont even have to be allergic to mold to have an attack.
- Pests: Cockroaches, mice and other household pests can cause asthma attacks.
- Pets: Your pets can cause asthma attacks. If youre allergic to pet dander , breathing in the dander can irritate your airways.
- Tobacco smoke: If you or someone in your home smokes, you have a higher risk of developing asthma. The best solution is to quit smoking.
- Strong chemicals or smells.
With asthma, you may not have all of these symptoms. You may have different signs at different times. And symptoms can change between asthma attacks.
Fatigue Can Occur After A Flare
Response from Theresa Cannizzarro, RT:
Yes! While fatigue isnt one of the more common asthma symptoms, it definitely can happen. When your body is working harder to breathe, it makes your body tired. Your body is having to compensate to bring more oxygenated blood from your lungs to the rest of your body so, in turn, you feel overall fatigued. Also, after a significant asthma flare-up, you may feel pretty fatigued for a period of time while your body recovers to its normal healthy state.1,2
Recommended Reading: How To Make A Homemade Inhaler For Asthma
When To Use A Vaporizer Humidifier Or Nebulizer
When choosing between a nebulizer, humidifier, or vaporizer, knowing their purpose and capabilities is essential. Among other things, each device will reduce discomfort this includes skin dryness, a dry nose, or prickly throat.
These devices also make it easier to breathe by reducing nasal congestion. Here are some pointers on when to use a nebulizer, humidifier, or vaporizer:
During Allergies
The most common symptom of allergy is congestion in the nose or chest. Therefore, humidifiers and vaporizers help increase the humidity in the air by adding moisture.
Inhaling moist air can help reduce the stuffiness in your nose and provide relief to your irritated sinus.
However, using these devices also comes along with certain precautions. If the humidity level is set too high, it can result in mold and dust mites, which are the most prevalent triggers for allergies.
Similarly, lower humidity is also harmful therefore, it is best to achieve the optimum level.
However, according to the American Academy of Asthma, Allergy, and Immunology, people with indoor allergies must first consult their doctors before buying any humidifier.
A vaporizer, however, is a better option for someone who has indoor allergies since the mist they create is heated, lowering the presence of contaminants is lowered.
Asthmatic Problems
Much like someone with allergies, a person with asthma should also be cautious when using a humidifier or vaporizer.
Are Nebulizers Ok To Use At Home
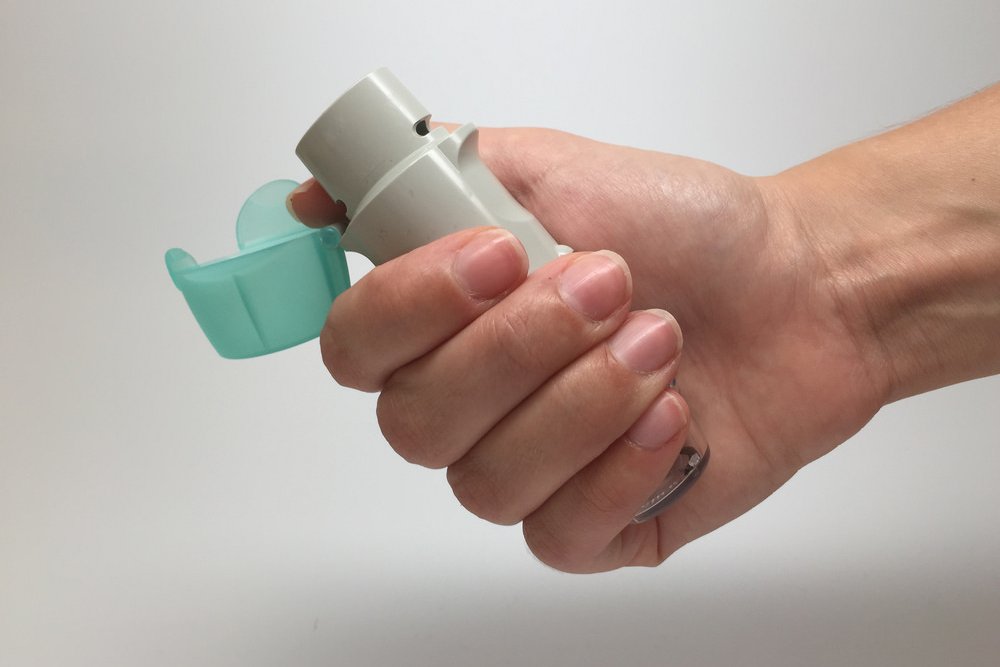
Sometimes patients have difficulty using handheld inhalers and instead use nebulizers, which turn liquid medicine into a mist. Particularly when the patient is experiencing severe asthma symptoms, nebulizers can be more effective at delivering medication slowly into the airways.
The current concern about nebulizers is that if they are used by a patient with a respiratory infection, the nebulizer could aerosolize droplets containing virus, allowing the virus to stay in the air longer. Hospitals and other facilities are being advised to reduce their use of nebulizers to reduce spread of the new coronavirus.
If an asthma patient finds that nebulized therapy is more effective than inhalers, the nebulizer should be used in a room that is isolated from other household members.
Read Also: Does Weight Gain Make Asthma Worse
What If My Child Skips A Dose Of Quick
Quick-relief medicines work immediately to handle the symptoms of asthma flare-ups when they happen. These medicines often are inhaled directly into the lungs. Within minutes, they open up the airways and relieve symptoms like wheezing, coughing, and shortness of breath.
Not taking quick-relief medicines during an asthma flare-up can be very harmful. A child might not be able to take a deep breath, and the airways can continue to tighten until the child must go to the ER.
Make sure your child always has quick-relief medicine handy in case of an emergency.
Pay Attention To Your Symptoms
I want to really stress that symptoms trump numbers. I’ll say it again: SYMPTOMS TRUMP NUMBERS. If you are having difficulty breathing, consider that before the number you see on a screen. I teach new respiratory therapists, nurses, and interns that you always treat the patient and not the numbers you see.
While pulse oximeters are great and can be a handy little tool for asthma monitoring, knowing exactly what they do and their limitations can be helpful.
Read Also: Eu Natural Breathe Side Effects
Why Is My Reliever Inhaler Not Enough
Reliever inhalers relax your airways, which help breathlessness, but they do not treat airway inflammation. As well as the relaxing effect of a reliever inhaler, you need the anti-inflammatory effect of a preventer. Once airways are less inflamed, they are less sensitive to triggers such as cigarette smoke and viral infections.
What Are Safe Inhalers For Glaucoma
Dear Dr. Mahler:What is a safe inhaler medication for my ASTHMA/Centrilobular Emphysema who also has closed angle glaucoma?Darlene from Tulsa, OK
Diagram shows overlap between asthma and COPD
25%Treatment for Both Asthma and EmphysemaTypes of Glaucomaopen angleclosed or narrow angle
In a healthy eye, excess fluid leaves the eye through the drainage angle, keeping pressure stable.
should be used with caution in patients with narrow angle glaucoma.DarlenePlease note, the advice provided is not a substitute for asking your health care professional about your specific situation.
Also Check: What Happens If You Smoke Weed With Asthma
When You Should Pack Your Portable Nebulizer
The last thing you want is to be without your breathing treatment when you need it most. If you plan on traveling on an airplane and any of these situations apply to you, then you should pack your portable nebulizer in your luggage.
- You recently had a flare-up: If you have recently had a flare-up of your COPD or asthma or other chronic respiratory condition, it would be wise of you to bring your portable nebulizer machine. This will ensure that you have access to treatment when you need it most.
- The time of year: If you know that you are susceptible to breathing symptoms during a certain time of year, you should take your treatment with you anytime you travel during that time.
- You will be gone for an extended time: An extended time can vary from person to person and how often they normally use treatment. If you regularly use your nebulizer for breathing treatments, you should consider bringing it.
You should always air on the side of caution and bring your nebulizer if you think you will need it. Even if you do not end up using it, it is better to be safe than sorry.
Fatigue And Asthma May Coexist
Response from Lorene Alba, AE-C:
Fatigue can be associated with asthma in many ways. Feeling tired can be an early warning sign that an asthma episode may be coming. Since asthma can worsen at night, symptoms can keep you from getting a good nights sleep. Fatigue is also common after having an asthma episode, so you may feel tired or even exhausted for several days or more.2
Also Check: Can You Be In The Military With Asthma
Side Effects Of Steroid Tablets
Oral steroids carry a risk if they are taken for more than three months or if they are taken frequently . Side effects can include:
- easy bruising
- muscle weakness
With the exception of increased appetite, which is very commonly experienced by people taking oral steroids, most of these unwanted effects are uncommon.
However, it is a good idea to keep an eye out for them regularly, especially side effects that are not immediately obvious, such as high blood pressure, thinning of the bones, diabetes and glaucoma.
You will need regular appointments to check for these.
Want to know more?
How Is Your Reliever Inhaler Different To Your Preventer Inhaler

-
Your reliever inhaler is usually blue. You only use it when your symptoms are getting worse or youre having an asthma attack. Your reliever inhaler treats asthma symptoms quickly when they come on.
-
Your preventer inhaler comes in different colours. You use it every day as prescribed to prevent asthma symptoms. Your preventer inhaler keeps down the inflammation and sensitivity in your airways.
Did you know? If youre regularly using your reliever inhaler, and relying on it to manage symptoms, youre more at risk of an asthma attack.
This is because your reliever doesnt deal with the underlying inflammation in your airways.
See your GP or asthma nurse to talk about managing your asthma better with a good preventer inhaler routine.
Recommended Reading: Does A Dehumidifier Help With Asthma
