The Discovery Of Ige And Its Role In Allergic Inflammation
While the discovery of IgE in 1966 brought to an end the search for the elusive reagin, it unlocked an era of discovery that investigated the genetics, structure, functions and clinical applications of this immunoglobulin . As has been recognised since the early part of the twentieth century, IgE has unique properties among the immunoglobulin isotypes in its abilities both to induce extremely rapid pathological responses and to act as a highly sensitive immunological amplifier. Furthermore, it is well established that IgE levels are increased in patients affected by atopic conditions and that IgE provides the critical link between the antigen recognition role of the adaptive immune system and the effector functions of mast cells and basophils at mucosal and cutaneous sites of environmental exposure . These functions have made IgE an attractive target for pharmacological intervention with IgE blockade having clinical potential across many different therapy areas.
Can Asthma Reappear In Adults After Disappearing Years Ago
Asthma is usually diagnosed in childhood. In many patients however, the symptoms will disappear or are significantly reduced after puberty. After age 20, symptoms may begin to reappear.
Researchers have tracked this tendency for reappearing asthma and found that people with childhood asthma tend to experience reappearing symptoms through their 30s and 40s at various levels of severity.
Regardless of whether your asthma is active, you should continue to avoid your known triggers and keep your rescue medications or prescriptions up-to-date and handy in case you need them.
In this section: Diagnosis and Lung Testing | How To Tell You Have Asthma | Your Healthcare Team
Asthma is a complex disease to diagnose, and only a healthcare professional is able to make a proper diagnosis.
If you are concerned that you may have asthma, contact your healthcare provider. In order to confirm an asthma diagnosis, your healthcare provider will take into account your medical and family history, allergies, and conduct lung function testing such as spirometry.
Asthma Control During The Outcome Year
A greater percentage of patients with 1 BEC > 300 cells/µL experienced 1 severe asthma exacerbation during the outcome year compared with the never high group . Other measures of asthma control were not appreciably different among blood eosinophil pattern groups. Full asthma control was achieved by 22.3%, 24.3%, and 23.6% of patients in the persistently high, intermittently high, and never high groups, respectively.
|
Table 4 Asthma Control During the Outcome Year by Longitudinal Eosinophil Pattern |
|
Table 5 Association Between Eosinophil Pattern and the Rate of Exacerbations During the Outcome Year |
|
Figure 4 Association between longitudinal eosinophil patterns and exacerbations in the outcome year by smoking status. Abbreviation: CI, confidence interval. |
Read Also: Asthma Inhaler Ingredients
Agents Targeting Corticosteroid Resistance
Several mechanisms that may account for corticosteroid-resistant asthma have been reported including activation of p38 mitogen-activated protein kinase and inflammatory genes regulated through transcription factor nuclear factor-B. P38 mitogen-activated protein kinase is important in the activation of GATA3, the master Th2 cytokine transcription factor. Small molecule p38 inhibitors have been demonstrated to attenuate asthmatic features in mice. However, clinical trials in humans for the treatment of inflammatory disease have been associated with substantial systemic side effects. Phosphoinositide 3-kinase also regulates inflammatory pathways, and activation of the isozyme PI3K by oxidative stress may decrease corticosteroid responsiveness through reductions in histone deacetylase 2, an enzyme targeted by theophylline. Other mechanisms for steroid-refractory asthma may include increased expression of the alternatively spliced variant of the glucocorticoid receptor and increased production of macrophage migratory inhibitory factor, which may block the anti-inflammatory effects of corticosteroids.,
Read Also: What Happens If You Smoke Weed With Asthma
Will This Diagnosis Change How My Asthma Is Treated

Maybe. Some patients with eosinophilic asthma respond to the traditional methods of treating it, using inhaled corticosteroids to reduce inflammation and bronchodilators like as a quick-acting rescue medication. However, since eosinophilic asthma affects the entire respiratory tract, inhaled steroids are often not enough, and many patients require systemic oral steroids to see symptom improvement.
New treatments are also being developed to reduce the number of eosinophils in the airway. These may be a good option for you if your symptoms dont respond to steroids.
-
Anti-interleukin-5 therapy- Interleukin-5 is a protein that activates eosinophils. Biologic therapies, such as mepolizumab and reslizumab , block IL-5. They are both used in conjunction with other asthma medications.
-
Anti-immunoglobulin E therapy- Immunoglobulin E is an antibody that plays a role in . Therapies, like omalizumab , that block IgE decrease both inflammation and the number of eosinophils in the airway. However, this treatment will only be effective for cases of eosinophilic asthma that are triggered by allergens.
-
Clinical trials- Researchers are studying other treatments that target interleukins, such as anti-IL-4 and anti-IL-13. Early results look favorable for these new therapies.
Read Also: What Can Cause Asthma Like Symptoms
Data Source And Study Design
Data were extracted from the Optimum Patient Care Research Database and the Clinical Practice Research Datalink GOLD database. OPCRD comprises data obtained through the Optimum Patient Care Quality Improvement services, which contains information from both anonymized electronic medical records and patient responses to disease-specific questionnaires. At data extraction, OPCRD contained data for approximately 10 million patients from more than 700 practices in the UK. CPRD GOLD is a primary care database of anonymized medical records that includes data for more than 11 million patients from 674 general practices in the UK.27 Data obtained from CPRD were limited to patients whose records could be linked to Hospital Episode Statistics, a comprehensive source for hospital admission and outpatient HCRU data. Patient-level data from OPCRD and CRPD are de-identified at the source, and patients have the option to opt-out of sharing their health information.
Baseline data represented the 12 months prior to the index date, defined as the most recent BEC measurement for which there were 12 months of subsequent outcomes data . Asthma outcomes and HCRU were evaluated for 12 months after the index date . The year of the index date for patients included in the data sets ranged from 2006 to 2018.
Other Tests You May Need If You Have Asthma
Even if your lung function tests are normal, your doctor may order other tests to see what could be causing your asthma symptoms.
- Gas and diffusion tests can measure how well your blood absorbs oxygen and other gases from the air you breathe. You breathe in a small amount of a gas, hold your breath, then blow out. The gas you exhale is analyzed to see how much your blood has absorbed.
- X-rays may tell if there are any other problems with your lungs, or if asthma is causing your symptoms. High-energy radiation creates a picture of your lungs. You may be asked to briefly hold your breath while you stand in front of the X-ray machine.
Recommended Reading: Does Walmart Sell Over The Counter Inhalers
You May Like: Can You Od On Albuterol
It Can Take Time To Get A Severe Asthma Diagnosis
Many people with severe asthma have already had asthma for some time and have tried different combinations of drugs. Just as theres no one-off test to diagnose asthma instantly, theres no single test to find out if the type of asthma you have is severe asthma. This means it can take time to get a diagnosis. The process and length of time will vary from person to person.
You can call our Helpline and speak to one of our respiratory nurse specialists on 0300 222 5800 or message them via WhatsApp on 07378 606 728 to ask any questions you have about your new diagnosis.
Next review due June 2022
What Does It Mean When You Have High Eosinophil Count
High levels of Eosinophils or high eosinophils counts in the blood is also known as Eosinophilia. This level ranges between 500 to 1500 per microliter of blood. A high eosinophils count may indicate a number of conditions, such as, allergies, asthma, inflammatory conditions like, Celiac disease or Inflammatory bowel disease, abnormal blood clells or Hypereosinophilic myeloid neoplasms, Eczema or dermatitis or other inflammatory skin conditions, parasitic infections, reactions to medications, or Cancerous growth including Hodgkins disease.
There may be a high level of eosinophils not only in the blood, but also in the bodys tissues. Because an underlying condition causes high eosinophils count, having high levels of eosinophols can cause several symptoms in a person. One must talk to doctor in such case and find out professional ways to treat eosinophilia.
Also Check: Fluticasone Side Effects Anxiety
Prep Procedure And Result Interpretation Of Aec Test
First and foremost, there is no need for any special preparation for the test. Just inform the physician if youre having any blood-thinning drugs like warfarin . Apart from these a few drugs need to be forgone before the test. Your doctor will advise you to stop taking certain medications.
Medications to avoid include diet pills, interferon, a few kinds of antibiotics, laxatives having psyllium, and tranquilizers. Also, ensure your doctor knows all the medicines that you are taking both current and very recent.
Once you are done with saying these a technician will draw a sample of blood which will be sent for further examination. The blood is drawn using a needle.
Following the result, if you get normal results it means you have fewer than 500 eosinophil cells per microliter of blood however, in children it varies depending on age.
In case, you have above 500 eosinophil cells per microliter of blood which is known as eosinophilia- a kind of disorder that is again the onset of many conditions.
If theres an unusually low eosinophil count it can be due to intoxication or the disproportionate creation of cortisol.
This in brief is what an absolute eosinophil count blood test is all about.
How Is An Asthma Flare
The best thing to do first if your asthma symptoms are getting worse is to use your rescue or quick-relief medicine. Ask your doctor if youre not sure what to use for quick-relief medicine. The usual inhaler dose is two to four puffs every 20 minutes for a total of three doses, or one nebulizer treatment if you have a home nebulizer.
You should be able to tell how serious the flare-up is after you use your quick-relief medicine. If you have a peak flow meter, check your PEF again after you use the quick-relief medicine. If your PEF is still very low, your flare-up is serious.
Your doctor may have given you a written Asthma Action Plan with directions for treating mild, moderate and severe flare-ups. If you dont have an action plan, ask your doctor for written directions about treating asthma flare-ups. If you have the symptoms of a serious flare-up or if your PEF is less than 50 percent of your personal best, call your doctor right away or go directly to the nearest hospital emergency room .
Don’t Miss: How To Treat Asthma Attack Without An Inhaler
Types Of Severe Asthma
There are two main categories of severe asthma Type-2 inflammation and Non-Type-2 inflammation. These categories are based on a persons response to treatment. Type-2 inflammation includes allergic asthma and eosinophilic asthma and Non-Type-2 inflammation includes non-eosinophilic asthma. For example, allergic asthma and e-asthma respond to treatment with inhaled corticosteroids and IgE -directed therapy or other biologics listed in the above table. Patients with Non-Type-2 inflammation, including non-eosinophilic asthma, generally do not respond well to inhaled corticosteroids. Allergic asthma and e-asthma have distinct biomarkers and treatment options available today. Treatments for non-eosinophilic asthma are currently being development.
Allergic asthma is caused by exposure to allergens such as pollen, pet dander, molds, etc. Most people diagnosed with allergic asthma will also have a diagnosis of hay fever or rhinitis. For these patients, exposure to allergens causes the bodys immune system to produce immunoglobulin E, an antibody that attaches to certain cells and causes them to release chemicals creating an allergic reaction. When this happens, common symptoms are sneezing, itchy/watery eyes, severe allergic reactions , and increased airway sensitivity.
Non-eosinophilic asthma includes neutrophilic, smooth-muscle mediated and mixed cells. People in this subgroup have few to no eosinophils in test results, and do not respond well to inhaled corticosteroids.
Therapeutics In Eosinophilic Asthma
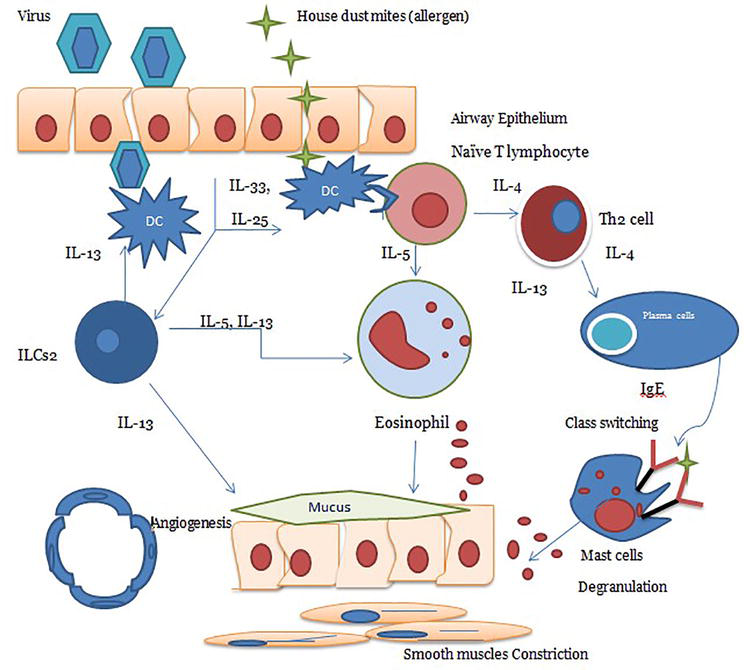
Current management of eosinophilic asthma begins with standard guideline-based therapy, including inhaled corticosteroids and bronchodilators which have been reviewed extensively elsewhere. Generally, the presence of eosinophils has been associated with responsiveness to corticosteroids although some patients with eosinophilic asthma have been reported to be steroid-refractory. Specific therapeutics targeting inflammatory mediators are currently under investigation in clinical trials for patients who have failed standard therapy and remain steroid-dependent or refractory.
Recommended Reading: What Happens If You Smoke Weed With Asthma
Role Of Innate Immune Activation
The common pathophysiological features of non-eosinophilic asthma involve an IL-8 mediated neutrophil influx and the subsequent neutrophil activation is a potent stimulus to increased airway hyperresponsiveness. Although the stimuli that trigger this response are diverse , the common features are consistent with activation of innate immune mechanisms rather than IgE mediated activation of acquired immunity. Recent data indicate a role for Toll-like receptors and CD14 in this process. TLRs can recognise a large variety of chemically diverse stimuli which then trigger proinflammatory responses involving NF-úB activation and chemokine production characteristic of non-eosinophilic asthma .
There is also the potential for combined activation of both innate and allergen specific inflammatory mechanisms to occur in asthma. This could result in a mixed eosinophil/neutrophil response as has been observed in some cases of acute asthma, and may explain the ability of ozone and NO2 to potentiate allergen induced asthmatic responses.
Recommended Reading: How To Get Rid Of Asthma Without Inhaler
Eosinophil Count In Sputum
The advance applications of methods to carefully and accurately induce and assess the sputum have allowed the possibilities to investigate the features of inflammatory process in airway in asthmatics. This brings attention to the heterogeneity of airway inflammation in asthma . Currently, sputum analysis is essentially an extensive and aseptic method for testing the airway inflammation. The analysis of sputum with hypertonic solution of saline is reliable in asthmatics who have just 0.9 L forced expiratory volume in the first second and is effective in almost 80% of asthma patients . The test for the collection, preparation, and determination of cell counts of sputum is easily characterized and organized, and its stability, responsiveness, and validity were explained. The normal values for sputum cell counts were determined, and on the basis of sputum examination, guidelines are available to improve the treatment. However, the eosinophil count in non-asthmatics is 1.2%, while 3% or more sputum eosinophil is usually believed as clinically important. Further investigation is required apart from the complete cell differentiation, probably the levels of biomarkers, like eosinophil-free granules, or the level of protein released from granules is precise and more significant .
Recommended Reading: Does Weight Gain Make Asthma Worse
What Does High Eos Absolute Blood Test Mean
High Absolute Eosinophils . A high absolute eosinophil count indicates that there is an elevated number of eosinophils a type of white blood cell in tissue or in the blood. Because white blood cells like eosinophils fight infection and cause inflammation, a high absolute eosinophil count may indicate a viral or bacterial infection, parasites,
Two New Medications For Severe Eosinophilic Asthma
Katherine Thompson, PharmD
CHI Health St. Elizabeth Regional Medical CenterLincoln, Nebraska
Lee E. Morrow, MD, MSc, FCCPProfessor of Medicine and Pharmacy PracticeCreighton UniversityDivision of Pulmonary, Critical Care, and Sleep MedicineOmaha, Nebraska
Professor of Pharmacy Practice and MedicineCreighton UniversityOmaha, Nebraska
US Pharm. 2017 42:16-19.
ABSTRACT: Asthma is a common, chronic respiratory disease in which the lungs airways become inflamed and narrowed. While the majority of patients with asthma can be treated effectively with the proper use of maintenance medications, patients with severe asthma are refractory to current standards of treatment, including oral corticosteroids. Eosinophilic asthma is a subset of severe asthma that is characterized by increased eosinophil counts. Because increased eosinophilia correlates with worse disease, mediators of the eosinophil pathway, such as interleukin-5 , are targets for preventing eosinophil-mediated inflammation. Recently, the new IL-5 receptor antagonists reslizumab and mepolizumab were approved by the FDA for use in severe eosinophilic asthma. Used as maintenance therapy, these agents may benefit patients with eosinophilic asthma.
Also Check: Does Ibuprofen Make Asthma Worse
Eosinophilic Asthma Blood Test
The number of eosinophils in a patients blood are measured. The blood draw is a simple, minimally-invasive procedure. It may be performed in a doctors office. People with eosinophilic asthma will have a high eosinophil count . High eosinophils with asthma does not always mean that a person has eosinophilic asthma. Other types of eosinophil-associated disease can cause too many eosinophils in the blood as well. Therefore, a doctor will interpret the results in context with a patients history, symptoms, and clinical exam.
Take The Asthma Control Test
The Asthma Control Test can help you and your doctor determine whether your asthma is being properly controlled. Share the score with your healthcare provider as a starting point for a conversation about your asthma management goals.
The Childhood Asthma Control Test* is a way to help your childs healthcare provider determine if your childs asthma symptoms are well controlled. Share the results with your childs healthcare provider.
Asthma Control Test is a trademark of QualityMetric Incorporated. *The Childhood Asthma Control Test was developed by GSK.
FREE Asthma Self-Care Guide
Better control starts now. Get yours.
GlaxoSmithKline believes your privacy is important. By providing your name, address, email address, and other information, you are giving GSK and companies working with GSK permission to market or advertise to you across multiple digital and offline channels, or contact you for market research or other purposes, regarding the medical condition in which you have expressed an interest, as well as other health-related information from GSK. GSK will not sell or transfer your name, address, or email address to any other party for their own marketing use. For additional information regarding how GSK handles your information, please see our privacy statement.
Read Also: What’s An Asthma Attack Feel Like
