First Principle: Deconstructing Airway Disease
Adverse stimuli can affect any biological tube in relatively limited and stereotypical ways. These are:
Narrowing to cause fixed obstruction
Narrowing to cause variable obstruction which changes spontaneously over time, and with treatment
Inflammation with various cell types predominant inflammation may be harmful or beneficial
The tube may become infected with combinations of bacterial, viral and fungal pathogens
There may be increased twitchiness of the tubethis is different from variable obstruction. An increased reflex expulsive effort may not be accompanied by transient airflow obstruction
The tube contents may be abnormal: including being too wet, too many solids, or too dry.
Furthermore, there are domains of risk, which also need to be considered in any discussion of pathophysiology:
Risk of acute asthma attacks, which may be fatal
Risk of impaired trajectories of lung growth, which may sometimes but not inevitably be associated with asthma attacks
risk of progressing from episodic wheeze to eosinophilic atopic school age asthma
A fourth risk, about which little is known and will not be discussed here, is the risk of failing to remit
Does the child have the treatable trait of eosinophilic airway inflammation which is likely to respond to inhaled corticosteroids ?
Does the child have the treatable trait of bacterial infection which is driving the disease and can be treated with antibiotics?
What Does Control Of Asthma Mean
- The ability to deal with acute exacerbations of asthma so that the need for urgent medical care is prevented
- Prevention of hospitalization for asthma
- Tolerating all normal activities up to and including competitive athletics if otherwise able
- The avoidance of symptoms that interfere with sleep.
- Normal pulmonary physiology .
- These goals should be reached safely and with the least interference with a normal life-style. The risks and bother of the treatment must be carefully weighed against the risk and bother of the asthma. The benefit obtained from the treatment must be worth any inconvenience and potential medication risks imposed by the treatment.
In other words, it is the goal of treatment to determine the simplest, safest therapeutic measures that minimize disability, normalize lung function, avoid the need for acute medical care of asthma, and permit a normal life.
What Body Systems Are Affected By Asthma
Fact Checked
Asthma is a chronic disease that affects your ability to breathe. Wheezing, breathlessness, chest tightness and coughing are common asthma symptoms. According to the Centers for Disease Control, an asthma attack or episode can affect your respiratory system, immune system and nervous system 1.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Don’t Miss: What Happens If Someone Without Asthma Use An Inhaler
How Will We Make Omics Work In Practice
When clinically indicated, invasive techniques can be used to discover novel mechanisms and pathways, but these will be only applicable in really severe cases, not in more mildly affected infants and children. For most cases, non-invasive approaches must be found, especially in children. Blood, urine and induced sputum can and should be routine clinical tests, there are other accessible biosamples which should be evaluated. Exhaled breath analysis is non-invasive, requires only passive co-operation, and with modern analytical techniques can give point of care answers. Investigators can distinguish different airway diseases in adults from a breathprint of VOCs . In children, 8 of 945 compounds studied could differentiate asthmatics from controls with a sensitivity of 89% and a specificity of 95% . There has been considerable interest in sophisticated mass spectrometry techniques, which can be applied for example to skin secretions, in order to detect airway infection in CF . The true test of the utility of these techniques will be whether they can differentiate children with non-specific respiratory symptoms from true asthmatics, and predict steroid responsiveness in the asthmatics. Perhaps in the future we will have a pediatric Breathalyzer which will give a readout of the important biomarkers to tell us the diagnosis, what endotypes are at play, and how best to treat the child.
Your Body Wants To Maintain A Certain Normal
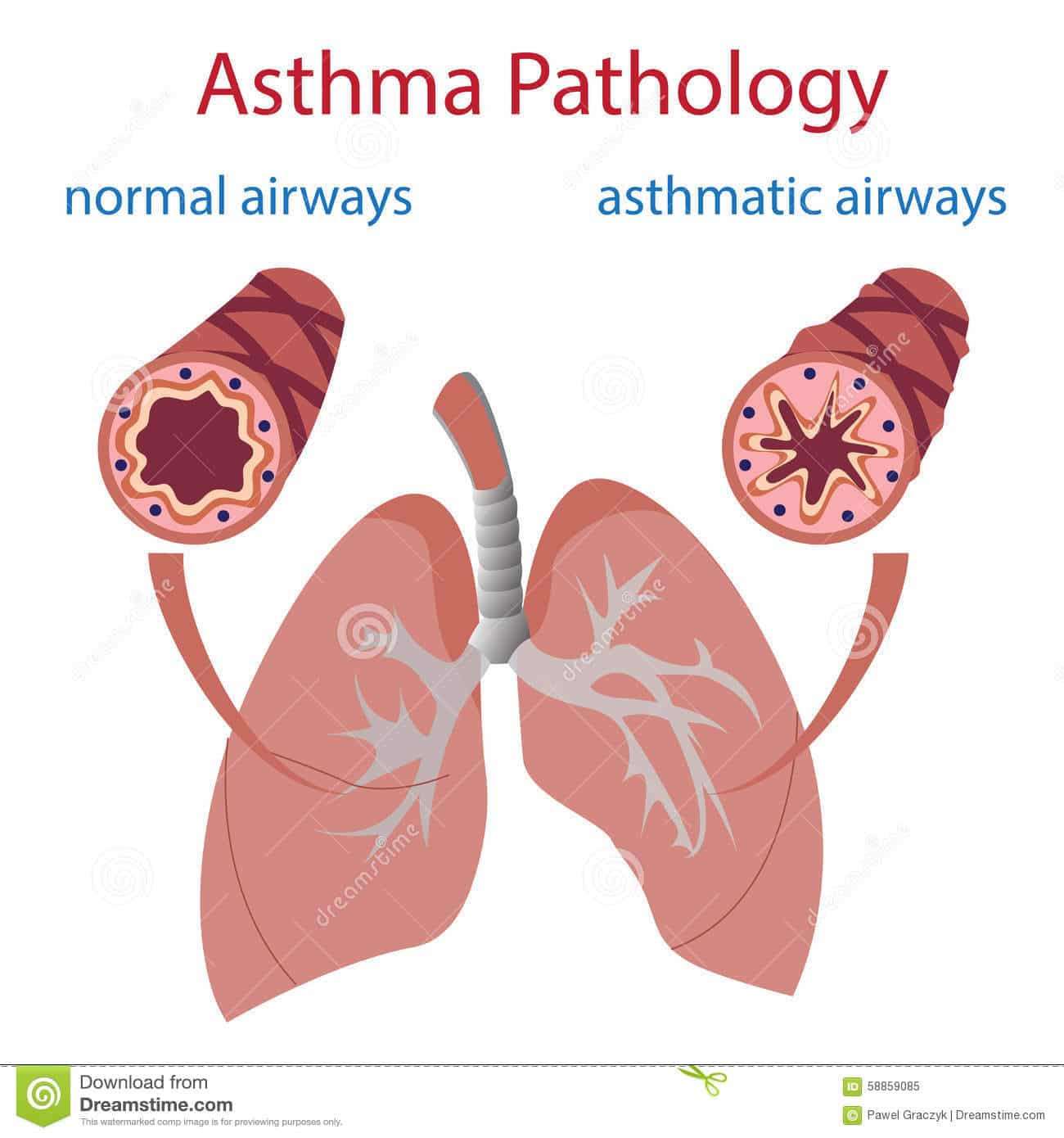
When you are outside and its raining, your body does a few things. First, a sensor detects whats going on in the world around you. When its raining, your sensor is your skin, and your skin tells your brain that its wet and cold out. Then, an internal mechanism reacts to that stimulus in this case, your brain helps raise your skin temperature by burning fat stores and calories youve consumed that day to help keep your body as warm as possible. When you are shivering, its actually a way for your body to warm itself up and increase circulation in order to keep your temperature high. In asthma the homeostasis of the smooth muscle in your lungs is interrupted when you are exposed to irritants such as dust or tobacco smoke or allergens such as pollen and symptoms can occur such as:
Once its stopped raining, your brain stops raising your body temperature with a negative feedback mechanism as a response to the fact that your body isnt experiencing the same stimuli. You stop shivering as soon as you arent as cold. And while some of those words and terms above might seem confusing, the way that all of it works is pretty straightforward. And its a perfect example of homeostasis. In asthma, it may take a rescue inhaler to revert the changes back or you may need to take a regular controller medication to try to keep homeostasis in balance.
Recommended Reading: What Is Prednisolone Used For In Asthma
What Triggers Asthma Symptoms
There are lots of things that can make asthma worse, but not everyone will be affected by the same things. Things that set off your asthma symptoms are called triggers.
Finding out what sets off your symptoms – whether it’s colds and viruses, pets, pollen, pollution, house dust mites, or stress – means you can work out ways to avoid your triggers if possible.
There are certain stages in your life that might affect your asthma too. For example, some women find that hormonal changes, at puberty, pregnancy, or menopause can affect their asthma.
The best way to cope with your asthma triggers is to always take your preventer medicine as prescribed, even when you feel well. And if you notice symptoms getting worse always see your GP or asthma nurse.
Does The Child With Another Pulmonary Or A Systemic Disease Also Have Asthma
Very frequently, ICS are prescribed to children with reasons other than asthma for being symptomatic, often either preceding the realization that a non-asthma disease is present, or on the just in case principle. This is to be deplored ICS have potential serious adverse events, not least the increased risk of pneumonia , tuberculous and non-tuberculous Mycobacterial infection , at least from adult studies.
Asthma in Other Pulmonary Diseases
The classical quandary is whether survivors of premature birth have asthma . Again, phenotyping resolves this. It is clear from a number of studies that these children have fixed and variable airflow obstruction . However, FeNO is normal not raised, even in the absence of ICS , nor is there an elevation of exhaled breath temperature , a non-specific sign of inflammation . Thus, unless there is evidence in a given individual of a second diagnosis of atopic, allergic asthma , ICS should not be prescribed. The same principles of investigation apply to other airway diseases, such as obliterative bronchiolitis and the airway disease after neuroendocrine cell hyperplasia of infancy these are discussed in detail elsewhere .
Asthma in Children With a Systemic Disease
Obesity AsthmaNot Lean Asthma in a Fat Body
Also Check: How To Stop Coughing Asthma Attack
What Does Asthma Do To The Body
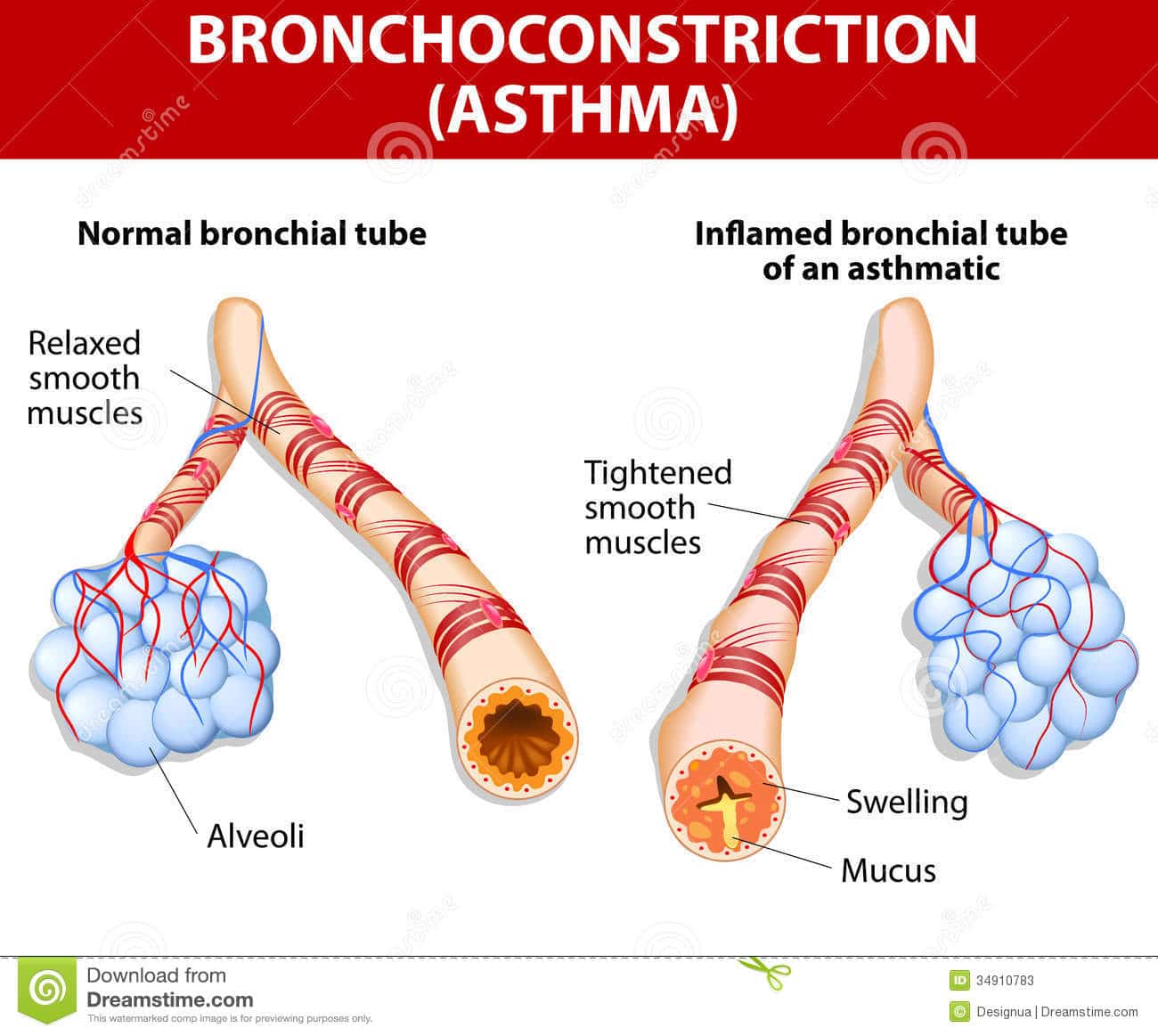
You already know that the muscles in your lungs tighten during an asthma episode. The bronchial tubes may become swollen or otherwise irritated. What else does asthma do to the body? Thats a great question.
According to American Academy of Allergy Asthma & Immunology, asthma causes a semi-permanent inflammation in the lungs airways. That means your airways are swollen and red. Theyre characterized as being in a hypersensitive state that can be irritated by any small trigger. Some of these triggers, outlined in Asthma Attacks: Triggers and Treatments, include pet dander, smoke, chemicals, dust, cold or warm weather, pollen, stress, and illness.
Unfortunately, its very normal for someone to be scared or fatigued after suffering an asthma attack. Even seconds of this frightening breathlessness can feel like hours, and your body needs time to recover from the shock of what happened.
Thats why you will have to take care of yourself in the days following an asthma attack. Your lungs are in a weakened state, which makes you more susceptible to a second or third attack. This risk is high over several days, so keep your asthma care a high priority.
What Is An Asthma Trigger
A trigger is anything that irritates your airways. Asthma is caused by two types of triggers.
- Allergic trigger: cause allergic reactions. Allergic triggers include things like dust mites, pollens, moulds, pet dander,
- Non-allergic trigger: are usually irritants. Non-allergic triggers include things like smoke, cold air, certain air pollutants, intense emotions
Learn more about different types of asthma triggers and how to manage them.
Read Also: How Do They Diagnose Asthma
Asthma Pathophysiology: Hypothesis Generating Studies
Gene expression is regulated in part by non-coding RNA, and this has been a subject of asthma research. In adults with severe asthma, activation status of CD4 and CD8 lymphocytes was related to non-coding RNA expression. There were significant changes in CD8 but not CD4 cells, Multiple pathways involved in T-cell activation were enhanced and there were many changes in miRNA expression . This is observational study, and very preliminary, but an important starting point. The rapidly expanding field of the role of micro-RNAs has been reviewed in detail elsewhere .
Mayo Research Examines How Asthma Affects Immune System Increasing Risk For Nonrespiratory Conditions
Young Juhn, M.D. , focuses his research on determining how asthma affects the immune system specifically, the extent to which asthma epidemiology affects the risk and severity of communicable and noncommunicable diseases. Asthma patients have a much higher risk of asthma-associated comorbidity including pneumococcal diseases, otitis media, community-acquired pneumonia, Streptococcus pyogenes upper respiratory infections, influenza, breakthrough chickenpox and pertussis, according to Dr. Juhns research.
This makes sense because these conditions are all airway infections, and asthma has an altered airway architecture including epithelial innate immune dysfunctions, says Dr. Juhn, director of the Asthma Epidemiology Research Unit at Mayo Clinic and a consultant in the Department of Pediatric and Adolescent Medicine. But we wanted to learn whether asthma patients susceptibility also applied to nonrespiratory conditions including systemic inflammatory and autoimmune diseases.
You May Like: What Does Asthma Sound Like
What Causes An Asthma Attack
An asthma attack can happen when you are exposed to asthma triggers. Your asthma triggers can be very different from someone elses asthma triggers. Know your triggers and learn how to avoid them. Watch out for an attack when you cant avoid your triggers. Some of the most common triggers are tobacco smoke, dust mites, outdoor air pollution, cockroach allergen, pets, mold, smoke from burning wood or grass, and infections like flu.
How Is Asthma Diagnosed
To diagnose asthma and distinguish it from other lung disorders, doctors rely on a combination of medical history, physical examination, and laboratory tests, which may include:
-
Spirometry. A spirometer is a device used by your doctor that assesses lung function. Spirometry is the evaluation of lung function with a spirometer. The test is performed by blowing as hard as possible into a tube connected to a small machine that measures the amount of air breathed out and in as well as the speed it is breathed out. This is one of the simplest, most common pulmonary function tests and may be necessary for any/all of the following reasons:
-
To determine how well the lungs receive, hold, and utilize air
-
To monitor a lung disease
-
To monitor the effectiveness of treatment
-
To determine the severity of a lung disease
-
To determine whether the lung disease is restrictive or obstructive
Peak flow monitoring . A device is used to measure the fastest speed in which a person can blow air out of the lungs. To use a peak flow meter, a person takes a deep breath in and then blows as hard and fast as possible into a mouthpiece. During an asthma or other respiratory flare-up, the large airways in the lungs slowly begin to narrow. This will slow the speed of air leaving the lungs and can be measured by a PFM. This measurement is very important in evaluating how well or how poorly the disease is being controlled.
Recommended Reading: Family Allergy And Asthma Clarksville Indiana
What Should I Do If I Have A Severe Asthma Attack
A severe asthma attack needs immediate medical care. The first step is your rescue inhaler. A rescue inhaler uses fast-acting medicines to open up your airways. Its different than your normal maintenance inhaler, which you use every day. You should only use the rescue inhaler in an emergency.
If your rescue inhaler doesnt help or you dont have it with you, go to the emergency department if you have:
- Anxiety or panic.
- Bluish fingernails, bluish lips or gray or whitish lips or gums .
- Chest pain or pressure.
Study Reveals Nervous Systems Role In Asthma Attacks
Asthma is a debilitating condition that kills 250,000 people around the world each year. People with asthma have hyperreactive airways and thickened lung walls obstructed with mucus. During an asthma attack, which could be fatal, airways constrict even further in the presence of a trigger, such as pollen, dust mites or a viral infection. Current asthma therapies treat asthma attacks as immune responses and focus on immune system suppression. However, a study by Dimitri Trankner of Howard Hughes Medical Institute in Virginia and his colleagues, published in the Proceedings of the National Academy of Sciences, shows that sensory neurons control bronchial hyperactivity.
Scientists know the immune system plays an important role in asthma. However, treatments that suppress the immune response and relieve inflammation do not control asthma symptoms completely. This indicates that asthma involves an additional mechanism.
Trankner and his team thought this mechanism might be nervous system activity. Sensory neurons in the vagal ganglia moderate respiratory responses such as coughing, and earlier studies have shown that the nervous system modulates asthma symptoms.
To test their hypothesis, the researchers genetically engineered mice with different groups of inactive neurons. They gave the mice an allergy to ovalbumin, egg white protein. This allergy causes asthma-like symptoms: airway hyperreactivity and constriction of the airways.
Explore further
You May Like: Does A Chihuahua Cure Asthma
What Is An Asthma Flare Up
An asthma flare-up is when asthma symptoms start up or get worse compared to usual. The symptoms wont go away by themselves and need treatment.
These flare-ups can happen quite quickly but they can also come on gradually over hours or days .
The term asthma attack is confusing because it means different things to different people from a bout of wheezing after running for the bus through to being admitted to hospital for asthma.
An asthma flare-up can become serious if not treated properly, even in someone whose asthma is usually mild or well controlled. A severe flare-up needs urgent treatment by a doctor or hospital emergency department.
Last reviewed Mar 2019
Does Asthma Cause Permanent Damage
The airway obstruction of asthma is generally completely reversible and usually does not cause permanent damage to the lungs, heart, or other organs. However, severe acute episodes of asthma can be associated with life threatening events and even fatalities. Survival of severe life threatening events can be associated with damage from lack of oxygen during the severe exacerbation, and lack of oxygen to the brain can cause loss of consciousness and brain damage.
Chronic asthma with ongoing airway inflammation may also be associated with what is called remodeling of the airways. This describes permanent changes occurring in the tissues surrounding the airways that results in permanent narrowing of airways. The potential for this emphasizes the importance of monitoring pulmonary function in patients with asthma at regular intervals, particularly those with a chronic pattern of asthma.
Dont Miss: Is Smoking Weed Bad For Asthmatics
You May Like: What Kinds Of Asthma Are There
Our Target: Endotyping The Airway
The general approach to airway endotyping has been to collect and characterize as far as possible large groups of patients, for example the U-BIOPRED and SARP cohorts, and use sophisticatedomics technologies to perform cluster analyses to try to determine the endotypes driving disease. However, caution is needed whether a child is in a particular cluster will be driven by the underlying endotype, but also the effects of adverse environmental, infective or other factors which may vary over time, the contrasting effects of prescribed treatment, and whether the treatment is actually used by the patient. Environmental factors are unstable over time, and changes may be dramatic . Treatment adherence is highly variable, difficult to measure and will affect the airway. Hence an eosinophilic airway may be the final common pathway of combinations of a steroid resistant endotype poor adherence to ICS treatment and increased environmental allergen exposure. Clearly the management of these three factors is very different. Very few groups have studied longitudinal stability of phenotypes or endotypes, and a second, validation cohort is rarely used when done, the evidence for stability is weak . Thus, our challenge is to differentiate what truly reflects a real endotype and what represents non-disease attributes . This is rarely addressed or even often identified as a problem.
Homeostasis As A Mechanism And A State
In the rain example above, we described homeostasis as a mechanism, or the way that your body reacts to a stimulus in order to achieve equilibrium. There are many different examples of homeostasis as a mechanism. Another good one is a fluid balance. Your body always wants to keep enough fluids on hand to keep all of your organs and processes running smoothly, but it will expel more fluids through waste when you drink more water in order to maintain healthy fluid levels. This is also important to asthma as dehydration can negatively impact your respiratory status, the mechanism by which your body senses how much fluid you have consumed, reacts to that, and then stops reacting once you have expelled enough, is an example of homeostasis as a mechanism.
However, theres a big caveat that throws off the what is homeostasis question. The term homeostasis can also be used as a state to refer to the equilibrium that your body is trying to achieve through the mechanisms discussed above. Homeostasis is the place your body wants to be its 98.6, fully hydrated, well nourished, and with all of the right vitamins and nutrients.
You May Like: Can Asthma Be Seen On A Chest X Ray
