What Is Good Asthma Care
Your doctor or nurse will tailor your asthma treatment to your symptoms. Sometimes you may need to be on higher levels of medication than at others.
You should be offered:
- care at your GP surgery provided by doctors and nurses trained in asthma management
- full information about your condition and how to control it
- involvement in making decisions about your treatment
- regular checks to ensure your asthma is under control and your treatment is right for you
- a written personal asthma action plan agreed with your doctor or nurse
It is also important that your GP or pharmacist teaches you how to properly use your inhaler, as this is an important part of good asthma care.
What Are The Treatments For Asthma
If you have asthma, you will work with your health care provider to create a treatment plan. The plan will include ways to manage your asthma symptoms and prevent asthma attacks. It will include:
- Strategies to avoid triggers. For example, if tobacco smoke is a trigger for you, you should not smoke or allow other people to smoke in your home or car.
- Short-term relief medicines, also called quick-relief medicines. They help prevent symptoms or relieve symptoms during an asthma attack. They include an inhaler to carry with you all the time. It may also include other types of medicines which work quickly to help open your airways.
- Control medicines. You take them every day to help prevent symptoms. They work by reducing airway inflammation and preventing narrowing of the airways.
If you have a severe attack and the short-term relief medicines do not work, you will need emergency care.
Your provider may adjust your treatment until asthma symptoms are controlled.
Sometimes asthma is severe and cannot be controlled with other treatments. If you are an adult with uncontrolled asthma, in some cases your provider might suggest bronchial thermoplasty. This is a procedure that uses heat to shrink the smooth muscle in the lungs. Shrinking the muscle reduces your airway’s ability to tighten and allows you to breathe more easily. The procedure has some risks, so it’s important to discuss them with your provider.
What Are The Risk Factors For Asthmatic Bronchitis
A number of factors that occur in conjunction with asthma increase the risk of bronchitis. Not all people with asthma who are exposed to risk factors will get asthmatic bronchitis, however.
Infection is usually the cause of asthmatic bronchitis.
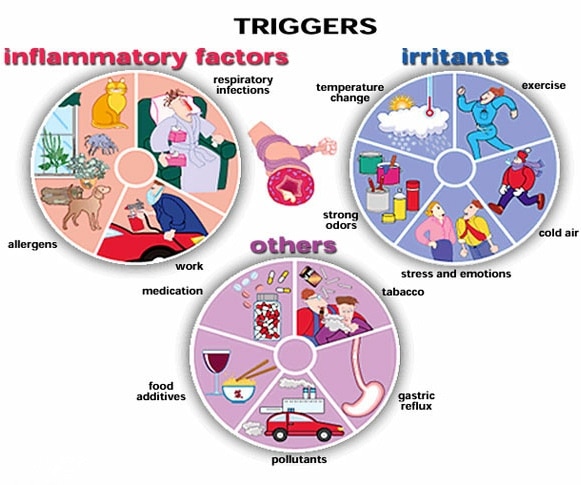
Risk factors or triggers for the exacerbation of asthma include:
Short-term asthma medications help in the event of an asthma attack.
Doctors do not tend to treat acute bronchitis with antibiotics, as the cause is usually a viral infection. Expectorants can help thin mucus in the airways, making it easier to cough it up.
Don’t Miss: What Test Do They Do For Asthma
How Do You Give Your Child Asthma Medication
You will be giving your child asthma medications using a valved holding chamber device or a home nebulizer .
Your child may be able to use a metered dose inhaler with a VHC. A VHC is a chamber that attaches to the MDI and holds the burst of medication. Talk with your child’s provider to see if an MDI with VHC is right for your child.
The nebulizer delivers asthma medications by changing them from a liquid to a mist. Your child gets the medicine by breathing it in through a facemask or mouthpiece.
There are some asthma medications that are also breath-actuated, or come as a dry powder. These medications are given to older children who are able to demonstrate the appropriate technique for using them.
Drug Discounts: A Consumers Guide To Cheaper Prescription Costs
The updated guidelines also recommend a type of drug called a long-acting muscarinic antagonist to improve symptoms for these age groups. And for young children who wheeze only when they have a respiratory tract infection , the new guidelines recommend a short course of inhaled corticosteroids plus a rescue inhaler as needed. This can prevent worsening of breathing problems and forestall the need for corticosteroid pills.
Most asthma medications are breathed in through the use of an inhaler or nebulizer. There are two main types of inhalers a metered dose inhaler , which uses a pressurized medicine-filled canister, and a dry powder inhaler , containing medicine in powdered form. A nebulizer uses a mask and delivers medication as a mist. Its important to learn the different techniques for using these devices to ensure the medicine reaches your lungs.
There are few evidence-backed natural remedies for asthma, particularly if your case is severe. But lifestyle changes, like controlling stress, and some complementary therapies, like acupuncture, may help manage symptoms.
You May Like: What To Avoid During Asthma
How Is Asthma Diagnosed
Your health care provider may use many tools to diagnose asthma:
- Medical history
- Lung function tests, including spirometry, to test how well your lungs work
- Tests to measure how your airways react to specific exposures. During this test, you inhale different concentrations of allergens or medicines that may tighten the muscles in your airways. Spirometry is done before and after the test.
- Peak expiratory flow tests to measure how fast you can blow air out using maximum effort
- Fractional exhaled nitric oxide tests to measure levels of nitric oxide in your breath when you breathe out. High levels of nitric oxide may mean that your lungs are inflamed.
- Allergy skin or blood tests, if you have a history of allergies. These tests check which allergens cause a reaction from your immune system.
Classification Of Bronchial Asthma In Etiology
Distinguish allergic and non-allergic forms of the disease. At children in 90-95% of cases there is an allergic / atopic bronchial asthma. Non-allergic forms of asthma are referred to as non-allergic. The search for specific causal environmental factors is important for the designation of elimination activities and in certain situations allergen-specific immunotherapy.
, , , , ,
Recommended Reading: How To Sleep With Asthma
Favorite Blogs About Living With Asthma
The Asthma Allergies Children blog is the work of two physicians, both trained in allergies and immunology. The blog covers topics like medication adherence, cost of care, doctors pet peeves, integrative medicine, new research, and other news. For timely takes on noteworthy topics, check it out.
Stephen Gaudet was born with severe asthma more than 60 years ago and started his blog back in 2004. The blog chronicles the trials and tribulations asthma has caused him, as well as the victories. To date, Gaudet has completed 21 races and nine marathons . Read more about his debilitating diagnosis and how he has overcome it.
Additional reporting bySari Harrar.
What Is A Peak Flow Meter And Why Use One
A peak flow meter measures how fast you can push air out of your lungs when you blow out as hard and as fast as you can. This is called peak flow.
Your peak flows measure how open the airways are in the lungs. Your peak flow may drop early even before you feel bad. This drop tells you that your asthma may be getting worse. Measuring your peak flow may help you learn what caused or triggered the drop, helps decide which medicines to add or take away and when you may need emergency care.
Don’t Miss: Can High Humidity Cause Asthma
Monitoring Asthma At Home
Some people use a handheld peak flow meter to evaluate their breathing and determine when they need intervention, before their symptoms become severe. People who experience frequent, severe asthma attacks should know how to reach help quickly.
Peak expiratory flow can be measured using a small handheld device called a peak flow meter. This test can be used at home to monitor the severity of asthma. Usually, peak flow rates are lowest between 4 AM and 6 AM and highest at 4 PM. However, more than a 30% difference in rates at these times is considered evidence of moderate to severe asthma. People with moderate to severe asthma, particularly those who need daily treatment to control symptoms, often use a peak flow meter to take measurements and compare them to their personal best to help identify signs of worsening asthma or the onset of an asthma attack.
All people with asthma should have a written treatment action plan that was devised in collaboration with their doctor. Such a plan allows them to take control of their own treatment and has been shown to decrease the number of times people need to seek care for asthma in the emergency department.
How Asthma Is Treated
While there is no cure for asthma, there are a number of treatments that can help control the condition.
Treatment is based on two important goals, which are:
- relieving symptoms
- preventing future symptoms and attacks
For most people, this will involve the occasional or, more commonly, daily use of medications, usually taken using an inhaler. However, identifying and avoiding possible triggers is also important.
You should have a personal asthma action plan agreed with your doctor or nurse that includes information about the medicines you need to take, how to recognise when your symptoms are getting worse, and what steps to take when they do so.
These symptoms are often worse at night and early in the morning, particularly if the condition is not well controlled. They may also develop or become worse in response to a certain trigger, such as exercise or exposure to an allergen.
Read our page on the causes of asthma for more information about potential triggers.
Speak to your GP if you think you or your child may have asthma. You should also talk to your doctor or asthma nurse if you have been diagnosed with asthma and you are finding it difficult to control the symptoms.
Recommended Reading: Is Zyrtec Good For Asthma
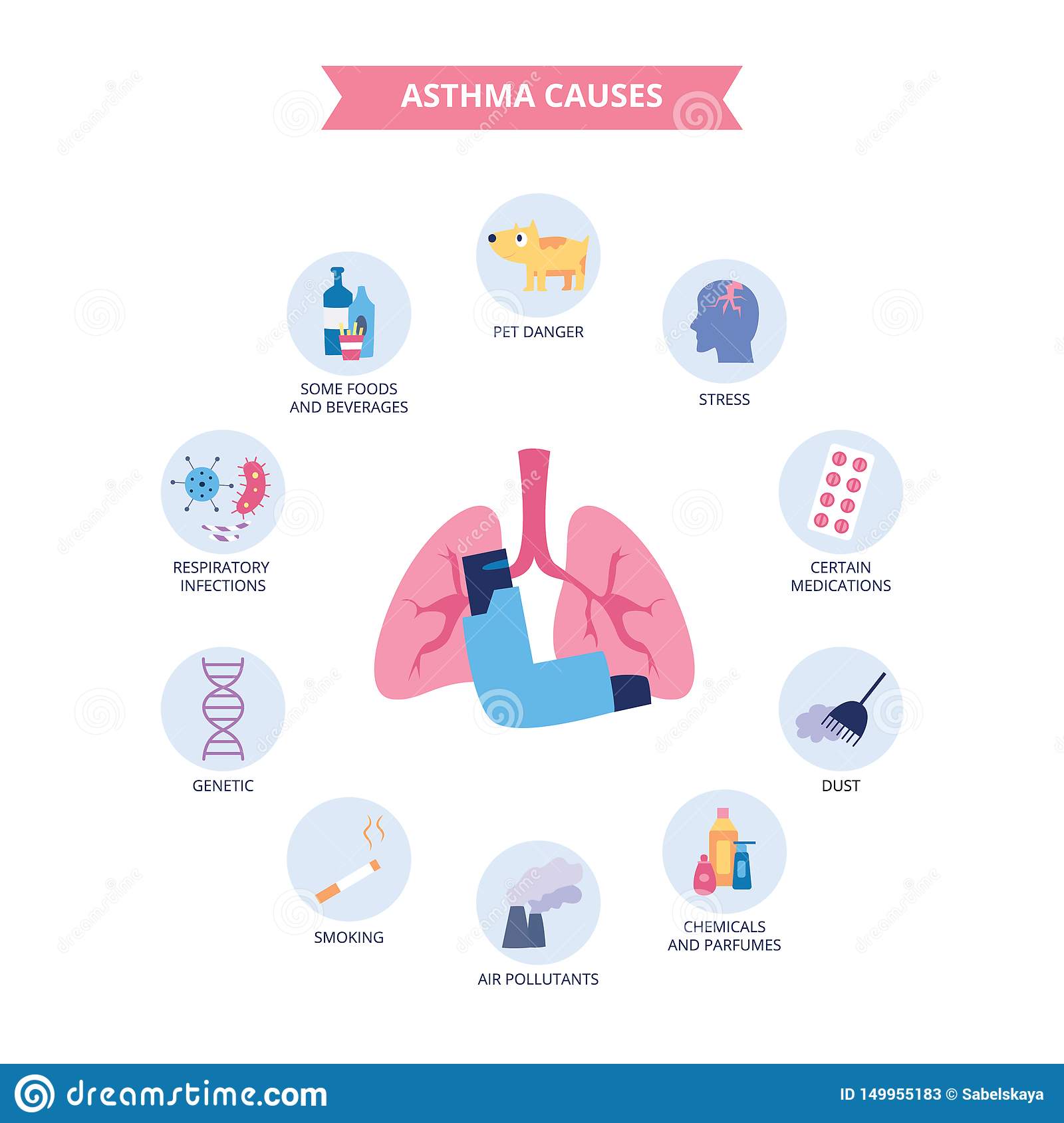
What Is An Asthma Trigger
A trigger is anything that irritates your airways. Asthma is caused by two types of triggers.
- Allergic trigger: cause allergic reactions. Allergic triggers include things like dust mites, pollens, moulds, pet dander,
- Non-allergic trigger: are usually irritants. Non-allergic triggers include things like smoke, cold air, certain air pollutants, intense emotions
Learn more about different types of asthma triggers and how to manage them.
How Do You Use Your Asthma Action Plan
Keeping a daily record of your peak flows and understanding how this relates to changes in asthma will help you to better manage asthma episodes. To help with understanding how this works, caregivers use the traffic light system.
Your Asthma Action Plan has three zones: green, yellow and red.
- Green zone: Your asthma is well-controlled. Peak flow is 80% to 100% of your personal best.
- Yellow zone: Your asthma is getting worse or is poorly controlled. Peak flow is 50% to 80% of your personal best.
- Red zone: Your asthma is severe. It requires emergency care. Peak flow is less than 50% of your personal best.
To find the number ranges for your Asthma Action Plan zones, multiply your personal best peak flow by 1.0 , 0.8 , and 0.5 . Record these ranges in your asthma diary so that you can refer to them easily.
For example, if your personal best peak flow is 400 LPM, the zones will be:
- Green zone: 320 LPM to 400 LPM .
- Yellow zone: 200 LPM to 320 LPM .
- Red zone: Less than 200 LPM .
If you are in the yellow or red zone, you will need to adjust your medicine according to your healthcare providers instructions. Youll use the peak flow values and symptoms to take action to get or stay healthy. Make sure you understand and can follow your Asthma Action Plan. If you have any questions, ask your healthcare provider for an explanation.
Don’t Miss: How To Run With Asthma
Why Are More Children Getting Asthma
No one really knows why more and more children are developing asthma. Suggestions include the following:
- Children are being exposed to more and more allergens such as dust, air pollution and second-hand smoke.
- Children aren’t exposed to enough childhood illnesses to build up their immune systems.
- Lower rates of breastfeeding have prevented important substances of the immune system from being passed on to babies.
Why Is My Asthma Worse At Night
Asthma that gets worse at night is sometimes called nighttime asthma or nocturnal asthma. There are no definite reasons that this happens, but there are some educated guesses. These include:
- The way you sleep: Sleeping on your back can result in mucus dripping into your throat or acid reflux coming back up from your stomach. Also, sleeping on your back puts pressure on your chest and lungs, which makes breathing more difficult. However, lying face down or on your side can put pressure on your lungs.
- Triggers in your bedroom and triggers that happen in the evening: You may find your blankets, sheets and pillows have dust mites, mold or pet hair on them. If youve been outside in the early evening, you may have brought pollen in with you.
- Medication side effects: Some drugs that treat asthma, such as steroids and montelukast, can affect your sleep.
- Air thats too hot or too cold: Hot air can cause airways to narrow when you breathe in. Cold air is an asthma trigger for some people.
- Lung function changes: Lung function lessens at night as a natural process.
- Asthma is poorly controlled during the day: Symptoms that arent controlled during the day wont be better at night. Its important to work with your provider to make sure your asthma symptoms are controlled both day and night. Treating nighttime symptoms is very important. Serious asthma attacks, and sometimes deaths, can happen at night.
Recommended Reading: Best Natural Remedy For Asthma
Causes And Types Of Asthma
An asthma diagnosis means you have chronic swelling and inflammation in the bronchioles. Also referred to as wheezing or bronchial asthma, this condition can run in families or be triggered by allergies and irritants.
There are different types of asthma, which are classified by the cause of the condition or what triggers symptoms.
Caring For Your Mdi And Chamber
For most MDIs, remove the canister and rinse the plastic holder with warm running water once a week to prevent the holes from getting clogged. Shake well and let air dry. There are some medications in which the inhaler cannot be removed from the holder. These usually need to be cleaned by wiping the mouthpiece with a cloth or cleaning with a dry cotton swab. Refer to the patient instructions that come with your inhaler.
Clean the chamber about once a week. Remove the soft ring at the end of the chamber. Soak the spacer in warm water with a mild detergent. Carefully clean and, rinse, and shake off excess water. Do not hand dry. Allow to completely air dry. Do not store the chamber in a plastic bag.
Recommended Reading: How To Treat Asthma Attack
Bronchitis Copd And Emphysema
Bronchitis is another common cause of bronchial spasms. Acute bronchitis can develop as a complication of a respiratory infection or cold. Its a temporary condition that can typically be treated with medications.
Chronic bronchitis is a long-term problem. Its one of the conditions that make up chronic obstructive pulmonary disease . COPD is a group of progressive lung diseases that make it harder for you to breathe.
Emphysema is another disease that falls under the umbrella of COPD. In this condition, the tiny air sacs in your lungs become damaged or destroyed. This impairs their ability to fill with air and deflate properly.
Smoking And Passive Smoking
According to modern concepts, smoking is one of the main factors affecting the occurrence and course of bronchial asthma. Tobacco smoke contains a large number of substances that have a toxic, irritant effect , a carcinogenic effect. In addition, tobacco smoke dramatically reduces the function of the local bronchopulmonary defense system, primarily the ciliary epithelium of the bronchial mucosa . Ultimately, inflammation of the mucous membrane, sensitization and hyperreactivity of the bronchi develops under the influence of tobacco smoke components, which contributes to the development of bronchial asthma. The same negative impact has also passive smoking – staying in a smoked room and inhaling tobacco smoke. “Passive smokers” absorb the same amount of nicotine and other toxic substances of tobacco smoke from the smoke-free air of the premises, as the active smoker. Passive smokers are also more likely to have food and pollen sensitization compared to people living in premises where no one smokes.
Also Check: Will Benadryl Help Allergic Asthma
What Are The Risk Factors For Bronchial Spasms
Youre at higher risk of developing asthma, a common cause of bronchial spasms, if you have another allergic condition. For example, if you have food allergy or eczema, youre more likely to develop asthma. Youre also more likely to experience it if you have a close relative with asthma or other allergic conditions.
Heavy smokers are at greater risk of developing asthma and most other lung problems, including acute bronchitis, chronic bronchitis, and emphysema. Inhaling secondhand smoke also increases your risk of these conditions. Frequent exposure to air pollution or chemicals in your home or workplace can also increase your chances of developing them.
Older adults, young children, and anyone whose immune system is impaired face greater chances of developing respiratory infections. These infections can lead to acute bronchitis and bronchial spasms.
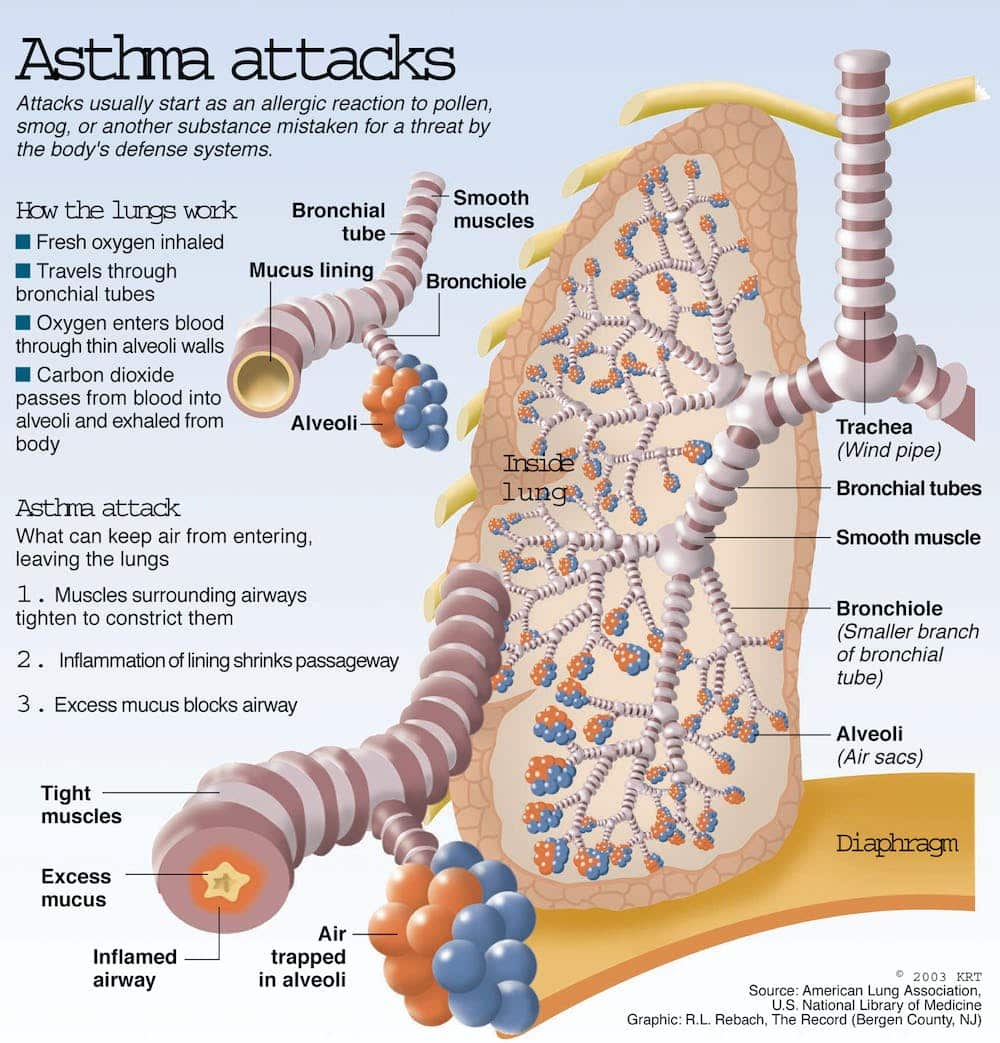
What Is Asthmatic Bronchitis
Asthmatic bronchitis refers to the incidence of acute bronchitis in a person with asthma. Acute bronchitis is a respiratory disease that causes inflammation in the bronchi, the passageways that move air into and out of the lungs. This inflammation results in respiratory congestion and shortness of breath. Asthma is a disorder that causes inflammation of the airways, leading to shortness of breath, chronic cough, chest tightness, and wheezing.
Acute bronchitis is a common respiratory disorder in the United States. Infants, young children, and elderly people have the highest risk of developing acute bronchitis. Acute bronchitis is commonly caused by upper respiratory viral infections. If you have asthma, your risk of acute bronchitis is increased because of an increased sensitivity to airway irritation and inflammation. Your risk of acute bronchitis is also increased if you smoke or are exposed to air pollution.
The signs and symptoms of asthmatic bronchitis vary among individuals, depending on the severity of the infection. Treatment for asthmatic bronchitis includes antibiotics, bronchodilators, anti-inflammatory drugs, and pulmonary hygiene techniques such as chest percussion and postural drainage .
Healthy lifestyle practices, including good hand washing, drinking plenty of fluids, following a well-balanced diet, getting plenty of rest, and avoid smoking, can help prevent or improve asthmatic bronchitis.
Also Check: Can Asthma Cause Chest Pain On One Side
