Causes And Triggers Of Childhood Asthma
Common triggers include:
- Airway infections. This includes colds, pneumonia, and sinus infections.
- Allergens. Your child might be allergic to things like cockroaches, dust mites, mold, pet dander, and pollen.
- Irritants. Things like air pollution, chemicals, cold air, odors, or smoke can bother their airways.
- Exercise. It can lead to wheezing, coughing, and a tight chest.
- Stress. It can make your child short of breath and worsen their symptoms.
Objective Measurement Of Airflow
Physicians’ estimates of response to therapy are often inaccurate in acute asthma. Failure of initial bronchodilator therapy to significantly improve the FEV1 or PEF is predictive of a more prolonged attack course or the need for hospital admission. The may correlate with PEF and, in some level III studies, correlates with the likelihood of admission. Low may indicate a need for admission to hospital, but normal levels do not exclude severe asthma or the possibility of relapse. Measurement of may help to guide treatment in adult patients, but no studies have shown that arterial blood gases or predict outcome.
When To Go To The Er If Your Child Has Asthma
One of the main goals of parents whose kids have asthma is avoiding trips to the emergency room for breathing problems. But its also important to know when going to the ER is the right choice.
Youll be better prepared to make that decision if you discuss it with your doctor before your child has a severe flare-up. The doctors instructions should be included in the asthma action plan. The plan will list specific symptoms that are your cue to go to the ER. If old enough, your child also should know what these signs are.
You May Like: Diy Nasal Inhaler
Face Masks And Spacer Devices
Most young children will be prescribed a face mask which attaches to their inhaler. Older children will be prescribed a ‘spacer device’. A spacer device is a plastic or metal container with a mouthpiece and a hole for the inhaler.
If your child has been prescribed a face mask or a spacer device, it is important to always use these. Face masks and spacers are the best way of making sure that your child gets the correct dose of medication right to their lungs.
Everyday Treatment For Asthma In Children
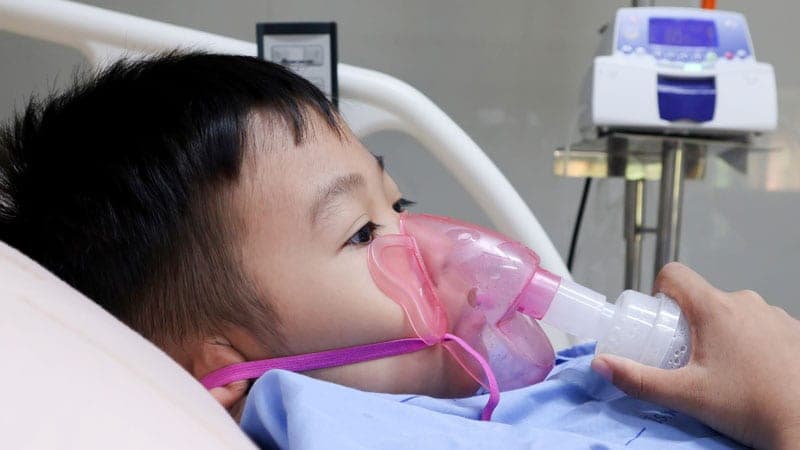
The main aims of day-to-day asthma treatment are to:;
- keep symptoms under control;
- keep lungs as healthy as possible;
- stop asthma from interfering with school or play;
- help your child enjoy a full and active life.;
Your doctor will help you to develop a plan to manage your childs asthma;which will include;an;asthma;action;plan;, and will prescribe the correct medication to help you do so.;
Don’t Miss: How To Take Care Of Asthma Without An Inhaler
Childhood Asthma Risk Factors
Asthma is the leading cause of long-term illness in children. It affects about 7 million kids in the United States. Those numbers have been going up, and experts arenât sure why.
Most children have their first symptoms by age 5. But asthma can begin at any age.
Things that can make a child more likely to have asthma include:
- Exposure to secondhand tobacco smoke before or after birth
- African-American or Puerto Rican descent
- Being raised in a low-income environment
Asthma Information For Childcare Kinder Or School
To assist;childcare and preschool workers and school teachers in the care of your child with asthma:;
- Tell them that your child has asthma .;
- Provide them with a copy of your childs asthma action plan, including emergency contact details. Make sure you provide an updated plan every year, or if your childs medication changes.The school or childcare centre will require this for enrolment.
- Show staff members how to use the medication devices, such as spacers and puffers.;
- Make sure your child has an up-to-date supply of medication and a spacer at the centre or school.;
- Notify staff if your childs asthma changes.;
- Tell the staff about any concerns you may have.;
Also Check: What Does A Nebulizer Do For Asthma
When To Go To The Hospital For An Allergic Asthma Attack
The first step in treating an allergic asthma attack is to use a rescue inhaler or other rescue medication. You should also move away from any source of allergens that might be triggering the attack.
If symptoms dont improve after using rescue medications, or you have severe symptoms, call for emergency medical help. In the United States, that means dialing 911 to call for an ambulance.
Severe asthma attacks share many symptoms with mild to moderate asthma attacks. The key difference is that the symptoms of a severe allergic asthma attack dont improve after taking rescue medication.
You might wonder how you can tell the difference between symptoms of a severe attack that requires emergency treatment versus a mild attack that you can treat on your own. Always seek emergency medical attention if your rescue medication doesnt seem to be working. You should go to the hospital if you notice any of these symptoms:
- intense shortness of breath and difficulty speaking
- very rapid breathing, coughing, or wheezing
- straining chest muscles and difficulty breathing
- a bluish color in the face, lips, or nails
- difficulty inhaling or exhaling completely
- gasping
- confusion or exhaustion
- fainting or collapsing
If you use a peak flow meter a device that measures your peak airflow you should go to the hospital if your readings are low and arent improving.
What Will Happen In Hospital
Most people who arrive at A&E with an asthma attack are treated first in the A&E department. And it may be that once you’ve been treated, and monitored for at least four hours, the A&E team will be happy to discharge you and you won’t need to stay in.;
If extra care is needed you may be admitted to;either the High Dependency Unit or Intensive Care;.;And once youre able to breathe more easily you may be transferred to a general ward to recover.
Your time on the ward is all about recovery
While youre on the general ward in hospital youll continue to be given reliever medicine either with a nebuliser, or an inhaler. You may be given;steroid tablets;to reduce the inflammation in your lungs.
The doctors and nurses will continue to monitor your progress, gradually lowering the amount of emergency medicines you needed when you first came into hospital, and regularly checking your peak flow to see how well youre recovering. You may also have further tests such as blood tests and chest X-rays.
If youve come to the ward from ICU, then an ICU nurse will usually check in on you while you stay in hospital. You may also be seen by a physiotherapist who will give you exercises to help strengthen all your breathing muscles and help you to control your breathing pattern so that you can breathe well on your own again, and avoid the risk of lung infections.;
Also Check: How To Prevent Asthma Symptoms
Does Your Child Have An Asthma Action Plan
Image Source
Were finally back to familiar schedules and routines now that school is in session, but leaving children in the care of other adults can be understandably frightening for the parents of asthmatics. Whether your child is in school, at football practice or on a field trip, the reigns have to be handed over to other adults who know your child and their asthma background.
Prior to the beginning of the school year, most children will visit their pediatrician, primary care provider or allergist/immunologist for their annual well-child appointment. Here, most asthmatic children will receive or review their existing asthma action plan. This well-outlined plan created by you and your physician is unique to your childs asthma, and will serve as a guide for all parties to use in preventing and reducing your childs asthma flare-ups and emergencies.
The asthma action plan should include most of the details youd expect, including possible triggers, early flare-up symptoms to look for, how to manage them with medication and who to reach out to for help should your childs health status become emergent, concerning or life-threatening.
Triggersare harmless to most people, but can bring about flare-ups for asthmatics. These commonly include:
- allergens
- change in weather
- irritants or pollutants in the air
- respiratory infections
- coughing
- labored breathing, or shortness of breath
- grunting
- audible wheezing
How to use an inhaler
What Is Childhood Asthma
Childhood asthma is the same lung disease adults get, but kids often have different symptoms. Doctors also call this pediatric asthma.
If your child has asthma, their lungs and airways can easily get inflamed when they have a cold or are around things like pollen. The symptoms may make it hard for your child to do everyday activities or sleep. Sometimes, an asthma attack can result in a trip to the hospital.
Thereâs no cure for asthma in children, but you can work with your childâs doctor to treat it and prevent damage to their growing lungs.
You May Like: Does Cold Weather Make Asthma Worse
When To Go To The Er For An Asthma Attack
Asthma
There are few things people take for granted as much as breathing. Its such an automatic act that unless someone is consciously aware of it, it goes unnoticed Until suddenly, you cant do it anymore, that is.
What does it mean to have an asthma attack? What are the risk factors? How can you learn to recognize an attack is on its way?
What Are The Symptoms Of Asthma In A Child

Symptoms can occur a bit differently in each child. Children with asthma have times when they have few, if any symptoms.;They also have times when symptoms flare up. Symptoms may include:
- Cough that is either constant or comes and goes
- Wheezing or whistling sound that is heard while your child is breathing
- Trouble breathing or shortness of breath while your child is active
- Chest tightness
- Cough at night
- Noisy breathing
The symptoms of asthma can be like other health conditions. Make sure your;child sees his or her healthcare provider for a diagnosis.
Read Also: How To Ease Asthma Without Inhaler
Recommended Reading: Treat Asthma Without Inhaler
How Can We Avoid A Trip To The Er
Well-managed asthma is rarely life-threatening. Taking asthma medicines as prescribed can help prevent severe asthma flare-ups and the need for emergency care.
Be sure to schedule and keep follow-up visits with your doctor and to track your child’s asthma.
It’s important to monitor your child’s asthma using the written asthma action plan your doctor helps you create. This plan will outline day-to-day treatment, symptoms to watch for, and step-by-step instructions to follow during a flare-up.
Taking asthma seriously and working to manage it can make it less likely that your child will need to go to the ER.
Vaping And Lung Damage
- Talk with your teen about the dangers of vaping.
- Vaping can cause severe lung damage. It can become permanent.
- Vaping can even cause death .
- Vaping tobacco also causes nicotine addiction.
- For these reasons, the legal age to purchase vaping products is 21 in the US.
- Encourage your teen to not start vaping or to give it up.
- Warning: home-made or street-purchased vaping solutions are the most dangerous.
Recommended Reading: Is Weed Good For Asthma
How Can I Avoid It
Try to stay away from whatever makes your symptoms worse. You should have regular checkups with your doctor to make sure your asthma is under control. Take your medicines as directed by your doctor and get refills before they run out. You should use a spacer with your inhaler to get the most from your medicine.
Having an asthma action plan can help you notice when your symptoms are getting worse. Your doctor can help you make a plan like this one: . Once you know what your personal best peak flow is, you can check it regularly and keep a flow chart to track your asthma.
You should get a flu shot every year to help avoid getting the flu. Your doctor may also tell you to get a pneumonia shot.
Asthma Patterns In Children
Every childs asthma is different. Some children have mild, occasional episodes of asthma or only show symptoms after;exercising, or when they have a;cold. Some experience daily symptoms, while others have symptoms continuously, which limit their level of activity.;
Each pattern of asthma requires a different treatment approach. It is important to remember that children can still have a;severe and even life-threatening attack, even if they generally have mild or occasional asthma.;
Don’t Miss: Inhaler Before Running
When To Take Your Child To Hospital
This article is designed to help you decide if you feel you need to attend hospital if your child is unwell with symptoms such as fever, cough, vomiting, abdominal pain, diarrhoea, and headache. These are symptoms that everyone experiences at some stage. But how do you know when to take your child to the emergency department? On the one hand you are worried something serious might be occurring but on the other hand you do not want to over react.; The following is a guide that helps decide whether to get emergency help
It is useful to understand how the emergency assessment ;works, and this might help with your decision. Assessing the child starts with observation.
What health professionals look for ABCD
ABCD stands for airways,; breathing, circulation and disability.; However in this instance A is often used for Alertness.; Its aim is to ensure the seriously ill child is not missed. This is what the triage nurse or primary care doctor will be assessing as a first impression. ;Once this has occurred the ;child will be categorised depending on how sick he or she appears.
1. A =;Alertness & Responsiveness; this is probably the most important observation. How is the child relating to the environment, his parents, and the health professionals. A child who does not move from the parents arms and is not particularly responsive will be triaged as requiring immediate assessment. ;However the child who appears alert, and interacting, will be triaged lower.
Supporting Patients With Severe Asthma
Our commitment to your childs overall health extends beyond our clinic walls. Our team takes a hands-on approach to assess each patients asthma triggers in their home. We partner with the Community Asthma Initiative and other services to provide in-home evaluations, and can also perform virtual home assessments. If needed, we will work with landlords to advocate for a safer and healthier living environment for all children.
We also partner with school nurses to guide them on assessing our patients and delivering medications for asthma in school. Since medication adherence is a key part of success with an asthma management plan, we provide advice and tips to help ensure your child is taking their asthma medication as directed. In addition, we provide an array of educational resources to help you support your childs treatment plan.
Also Check: Asthma Attack No Inhaler
The Role Of Asthma Action Plans
An Asthma Action Plan can help. It has green , yellow , and red zones that help you know how to treat your asthma. You can and fill it out with your doctor.
With my kids, we learned that sometimes it is best to let the hospital take over medical care for our kids. They are fully trained and have all of the equipment to monitor them.
For those of you with small children that have asthma, pay close attention to their symptoms! Have a plan of what to do if your kids have any of the symptoms listed above – whether to call your doctor, call 911 or head to the hospital.
What Are The Symptoms Of Asthma

Asthma causes difficulty breathing because of narrowed, mucus-filled airways. This may cause a child to have trouble breathing and/or develop a tight feeling in the chest. Other asthma symptoms include fast breathing, wheezing, coughing, or needing to use extra muscles in the neck, chest, or abdomen to bring air into the lungs.
Symptoms of asthma are not the same for everyone. Some children have symptoms nearly every day and need to take medications. Other children may only have occasional symptoms, one or two times a week. These people may only need medications when they have asthma symptoms.
Also Check: Asthma And Weight
Going To The Hospital For My Childs Asthma
Home » Experience Journals » Asthma » Going to the hospital for my childs Asthma
Toby had a fever and he was breathing very fast, so I called the pediatrician and said, Im bringing him in. Toby is kind of a trooper. When I picked him up he said, I want to go see Mindy shes the nurse practitioner in my pediatricians office shell give me medicine and Ill feel better.
I felt so helpless and scaredEvan had been crying a lot and been so fussy and cranky all day. By the end of the day I was at my wits end. I put him in his crib for a little while thinking he might just cry himself to sleep. After a little while though, when he didnt stop, I went up to get him and after I got him out, he kept hitching for breath, like you do when youve just been crying, except the hitching never stopped. I knew something was wrong, but I didnt know what it was. Of course, by this time his doctors office was closing and they told me it was probably an ear infection, and I could either wait until morning and bring him in or take him to the ER. I had almost convinced myself to wait until the morning who wants to spend hours at the ER for an ear infection?
He ended up being admitted, being diagnosed with pneumonia and staying two or three nights in the hospital. I still feel like crying when I think about it. I feel guilty about not recognizing the symptoms earlier in the day and thinking about how much discomfort he was in and I thought he was just cranky.
