What Underlying Conditions Does The Cdc Recommend For Vaccine Eligibility
According to the Centers for Disease Control and Prevention , âPeople aged 16 years and older who have underlying medical conditions that increase the risk of serious, life-threatening complications from COVID-19, should be among those offered COVID-19 vaccine first.â The underlying conditions that the CDC lists are:
However, states are not required to distribute the vaccine in order that these conditions are listed â so if youâre looking to find out when you can get vaccinated, youâll want to check your stateâs vaccine eligibility guidelines.
Officials Identify 6 Victims Killed When Tornado Struck Edwardsville Amazon Warehouse
Here’s a list of underlying health conditions eligible for the vaccine in Phase 1C:
Cancer , Cardiac, cardiovascular, and cerebrovascular disorders , Chronic Kidney Disease, Chronic respiratory disorders , Diabetes , Disability: physical, developmental, visual, hearing, or mental, Neurologic conditions , Down Syndrome, Immunocompromised state including from blood or bone marrow transplant, immune deficiencies, HIV, use of corticosteroids, or use of other immune weakening medicines, Liver disease , Pregnancy, Obesity: BMI 30 kg/m2, Schizophrenia spectrum disorders, Sickle Cell Disease, Thalassemia, persons with disabilities
Click here for a full list of who is eligible in Chicago’s Phase 1C
The list of qualifying high-risk medical conditions in Phase 1B Plus includes:
- Cancer
- Pulmonary Disease
- Sickle Cell Disease
Currently, much of the Chicago area remains under Phase 1B guidelines, which open up vaccinations to people age 65 years and older as well as “frontline essential workers,” including first responders, education workers like teachers and support staff, childcare workers, grocery store employees and postal service workers, among others. That’s in addition to the health care workers and long-term care facility staff and residents who were eligible in Phase 1A of the state’s rollout.
Those already eligible under Phases 1A and 1B will also remain eligible in 1C.
This article tagged under:
What Is Known About Cases Of Allergic Reactions To Covid
CDC conducted research on vaccine administration through the first two months the mRNA vaccines were made available to the general public.
- Through Jan. 24, 2021, there were 50 reported cases of anaphylaxis in the United States after 9,943,247 doses of the Pfizer/BioNTech vaccine, according to the latest data from CDCs Advisory Committee on Immunization Practices . This amounts to 5.0 cases of anaphylaxis per 1 million doses given.
- For the Moderna vaccine, through Jan. 24 there were 21 reported cases of anaphylaxis in the United States after 7,581,429 doses. This amounts to 2.8 cases of anaphylaxis per 1 million doses given.
In most of the cases, anaphylaxis occurred in people who had a prior history of allergies or allergic reactions. Most of the reactions occurred within 15 minutes after the vaccine was given. No cases resulted in death.
The reports of anaphylaxis should not deter anyone from seeking out the COVID-19 vaccine. The vaccines are very safe, and severe allergic reactions are rare, CDC says. Always keep with you two epinephrine auto-injectors if you are at risk for anaphylaxis.
CDC, the National Institute of Allergy and Infectious Diseases and the U.S. Food and Drug Administration are working with vaccine manufacturers to further research COVID-19 vaccines and severe allergies.
Also Check: Can You Join The Army If You Have Asthma
What Is Known About The Johnson & Johnson Vaccine And Allergic Reactions
In Johnson & Johnsons press release announcing FDA approval of its COVID-19 vaccine, it states:
There is a remote chance the Janssen COVID-19 Vaccine could cause a severe allergic reaction. A severe allergic reaction would usually occur within a few minutes to one hour after getting a dose of the Janssen COVID-19 Vaccine. For this reason, your vaccination provider may ask you to stay at the place where you received your vaccine for monitoring after vaccination.
Johnson & Johnson says you should not get its COVID-19 vaccine if you have had a severe allergic reaction to any ingredient in its vaccine.
Prior to vaccination, be sure to tell the vaccine provider if you have any allergies. You should also tell the vaccine provider if youre immunocompromised or youre on a medicine that affects your immune system.
Home Sleep Apnea Testing During Covid

Tate recommends that people with poor COVID-19 outcomes be evaluated for sleep apnea to help get to the root of their illness. But testing doesnt need to be reserved for people whove already contracted COVID-19. Anyone with signs of OSA should consider getting screened for the condition in order to prevent complications down the line. In fact, the evaluation is something that can be done at home.
Before the pandemic, sleep studies typically occurred in a lab. However, many sleep centers are now dispensing home sleep apnea test units through mail delivery or using a curbside pickup and return.
A HSAT will calculate the number of sleep apnea eventsbreathing pauses plus the number of periods of shallow breathinga person has per hour while sleeping.
- Mild: 5 to 14 apnea events in an hour
- Moderate: 15 to 29 apnea events in an hour
- Severe: 30 or more apnea events in an hour
AASM recommends the diagnosis of OSA, assessment of treatment efficacy, and treatment decisions not be based solely on automatically scored HSAT data, because the raw data must be reviewed and interpreted by a physician who is either board-certified in sleep medicine or overseen by a board-certified sleep medicine physician.
Many sleep specialists, like Tate, are using telehealth to ensure proper set-up of the HSAT, answer patient questions and concerns, and provide follow-up.
Also Check: Severe Asthma Exacerbations
Tips For Wearing A Face Mask With Asthma
The Public Health Agency of Canada currently recommends that Canadians wear non-medical face masks while in public spaces where physical distancing cannot be maintained such as on public transit, or at the grocery store.
Be sure to check your provincial or territorial authority for up-to-date guidance.
Wearing a face mask is NOT a substitute for physical distancing or frequent handwashing. Wearing a non-medical face mask is an extra measure that can be taken to protect those around you. When worn properly, a person wearing a non-medical mask can reduce the spread of their own infectious respiratory droplets.
Make sure you wear your mask properly. It should cover both your nose and mouth. If your mask gets soiled or wet, be sure to wash and dry it before wearing it again. You can read information about appropriate use of non-medical masks, and how to properly place, remove and clean a non-medical mask from the Public Health Agency of Canada.
The vast majority of people with asthma can wear a non-medical mask safely. If you are unable to wear a non-medical mask without experiencing breathing issues, do not wear a mask. Instead, make sure you are practicing physical distancing by maintaining a 2-metre distance. Schedule an appointment with your healthcare provider as soon as possible to go over your Asthma Action Plan and review your asthma symptoms and control. Your healthcare provider may suggest or ask you to consider other options to protect yourself.
How Can I Look After My Asthma During The Pandemic
One of the most important things you can do right now is to manage your asthma well. You should make sure that youre seeking help when you need it and trying to book your usual appointments .
Some routine appointments may have been postponed, such as annual reviews. But annual reviews are important to ensure your condition is managed as well as possible and lower your risk of an asthma attack. So do book an annual review as soon as you can.
Emergency care
If you are having an asthma attack, this is an emergency. You must follow the steps on your asthma action plan and get your usual emergency care, including going to A& E or calling 999 if you need to.
Care from your GP
Speak to your GP or asthma nurse if you are getting asthma symptoms three or more times a week.
Follow these four asthma management steps to help you keep well:
You May Like: How To Get Rid Of Asthma Without Inhaler
Whos Getting The Vaccine Next And When
The Expert Vaccine Allocation Panel is considering what criteria could be used for later stages of vaccine distribution. This webpage will be updated when those decisions are completed.
Spring 2021 is the best estimate of when vaccine will be available for the general public, but that may change. It depends on vaccine production and how quickly other vaccines become available.
Asthma And Your Risk Of Becoming Ill With Covid
How your asthma affects your risk of becoming ill with COVID-19 seems to be mainly linked to how well-controlled it is. People with well-controlled asthma that is not severe dont seem to be at higher risk of dying from COVID-19.
People at higher clinical risk are those who either:
- have severe asthma
- need regular or continuous oral steroids
- have a history of asthma attacks that have required an overnight stay in hospital.
As a result, many of these people will be in the clinically extremely vulnerable group.
However, if you have any type of asthma there is a small increase in the risk of needing to go to hospital if you get COVID-19. Although the risk of this happening is small, its still very important to manage your condition well.
Its also important to remember that your own level of risk is affected by many different interacting factors. Your asthma may play a part in your level of risk from coronavirus, but your risk is also affected by lots of other things too.
Public Health England has identified the main factors that increase the risk of catching and becoming seriously ill with coronavirus as:
- being older
- having an underlying health condition
- being a man
- your job your risk level is higher if you work outside your home and come in to contact with lots of people every day
- where you live – if lots of people in your area are infected with coronavirus, its more likely youll catch it. Find official coronavirus statistics for your area.
Don’t Miss: Can Allergies Cause Asthma Attacks
How Should People With Asthma Prep Before Getting The Vaccine
People with asthma should be excited to start their pathway towards immune protection, Stukus says. Other than that, individuals with asthma should be aware of the common side effects in case they need to plan for time off work the day after they receive their vaccine. Most expected adverse effects occur in the first 48 hours and are very mild and short-lived, Stukus explains.
Additional reporting by Quinn Phillips.
What Is A Cpap Machine
A CPAP machine is designed to use positive airway pressure to keep the airway open during sleep reducing instances of sleep apnea events and snoring while improving respiration. Users wear a face mask and receive pressurized air from a connected hose. It is considered the gold standard treatment for those diagnosed with sleep disorders.
Companies like Aeroflow Healthcare are in-network with Medicare, Medicaid, and most private insurance providers and can work with both your primary and supplemental or secondary insurance to save you unnecessary out-of-pocket fees on CPAP supplies whenever possible. On their website, Aeroflow recommends the following:
- Every 6 months: Replace headgear, chinstraps, non-disposable filters, and humidifier water chambers.
- Every 3 months: Replace masks and tubing.
- Every month: Replace full-face mask cushions
- Every 2 weeks: Replace cushions, pillows, and disposable filters
You May Like: Does Weight Gain Make Asthma Worse
Reducing Your Risk Of Catching And Spreading Covid
There are lots of ways you can reduce the risk of catching and spreading the coronavirus, including:
- following the government guidance for where you live or work
- meeting outside where possible, or keeping inside well ventilated
- getting vaccinated and encouraging friends and family to do the same
- getting a PCR test if you develop symptoms
- self-testing regularly with a lateral flow test if you dont have symptoms
- self-isolating if you get positive test results
- washing your hands often, using soap and warm water, or hand sanitiser
- wearing a face covering to help protect others.
Stop smoking
Coronavirus is a respiratory infection. If you smoke, you have an increased risk of contracting a respiratory infection and of having worse symptoms. This means that if you catch coronavirus, your symptoms may be worse than those of a non-smoker. Smokers also touch their mouth and face more, which increases the risk of transmitting the virus from hand to mouth.
Its important that if you smoke, you stop as soon as possible. As well as lowering your risk from coronavirus, your breathing becomes easier within days of stopping smoking.
Get advice on how to stop smoking.
Wear a face mask or face covering
We strongly encourage that everyone who can continues to wear a face covering in enclosed or crowded spaces.
We have more information and advice on wearing a face covering if you have asthma, including an exemption card if you can’t wear one.
Find the guidance for your area
When And Where Can I Get It In North Texas
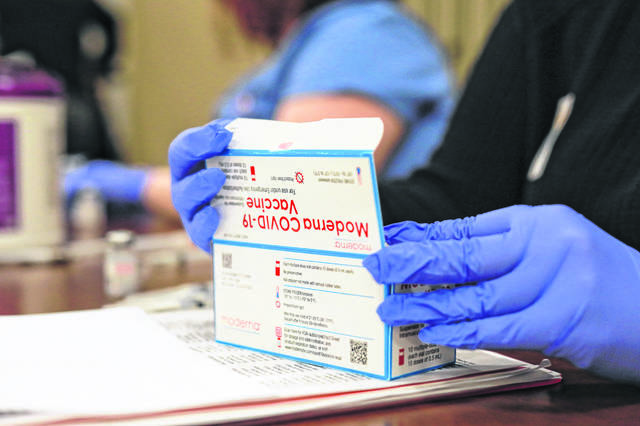
If you are included in the Phase 1B group, you can get the COVID-19 vaccine if your local provider has enough vaccine shots available.
On Jan. 10, Texas announced it was opening 28 large-scale hub locations. In addition, to reach smaller communities across the state, Abbott said vaccine doses would be delivered to 206 smaller locations. Go here for the list.
Dallas County is working to help vaccinate about 2,000 people per day from the site that opened at Fair Park on Monday, Jan 11.
To register for the COVID-19 vaccine, you can visit the Dallas County Health and Human Services website at .
Tarrant County Judge Glen Whitley said they would be registering residents from Ellis, Erath, Montague and Cooke counties. On Friday, Johnson County announced their residents would also be eligible to register in Tarrant County.
Dallas and Denton counties are also allowing people who are not residents to register for vaccinations.
Also Check: Albuterol Steroid Side Effects
Q& a With Aafa’s Medical Scientific Council
Now that the COVID-19 vaccine has reached the U.S., many people with asthma and allergies have questions about it. The Asthma and Allergy Foundation of America talked with three doctors on our Medical Scientific Council on Dec. 10, 2020, about the Pfizer-BioNTech COVID-19 vaccine. Please note this was recorded shortly before the FDA authorized the COVID-19 vaccines.
Here are a couple of the questions we asked the doctors and text excerpts from their answers. Please watch the videos below to hear their full answers.
Do I Need To Wear A Mask When I Get The Vaccine
Yes. The CDC recommends people wear a mask that covers their nose and mouth when in contact with others outside your household, when in healthcare facilities, and when receiving any vaccine, including a COVID-19 vaccine.
Anyone who has trouble breathing or is unable to remove a mask without assistance should not wear a mask. For more information, visit considerations for wearing masks.
Recommended Reading: What Is Small Airway Disease
What Are Some Reported Adverse Reactions To Each Vaccine
Pfizer: In clinical studies, adverse reactions in participants 16 years of age and older included pain at the injection site , fatigue , headache , muscle pain , chills , joint pain , fever , injection site swelling , injection ite redness , nausea , malaise , and lymphadenopathy .
Moderna: In clinical studies, the adverse reactions in participants 18 years of age and older were pain at the injection site , fatigue , headache , myalgia , arthralgia , chills , nausea/vomiting , axillary swelling/tenderness 19.8%), fever , swelling at the injection site , and erythema at the injection site .
What Do I Need To Do Now
- Phase 1A: If you are a healthcare worker, contact your employer. If you are a long-term care resident,contact your caretaker.
12/24/20- Only if the patient has PEG allergy should the patient be excluded. Here is the College’s guidance from our COVID-19 vaccine Task force:
American College of Allergy, Asthma, and Immunology Guidance on Risk of Allergic Reactions to the Pfizer-BioNTech COVID-19 VaccineDecember 14, 2020
Allergic reactions to vaccines, in general, are rare with the incidence of anaphylaxis estimated at 1.31 in 1 million doses given. With the emergency use authorization of the Pfizer-BioNTech COVID-19 vaccine by the FDA on December 11, 2020, the ACAAI COVID-19 Vaccine Task Force recommends the following guidance for physicians and other providers related to risk of an allergic reaction on vaccination. These recommendations are based on best knowledge to date but could change at any time, pending new information and further guidance from the FDA or CDC.
References:
Don’t Miss: Does Ibuprofen Make Asthma Worse
