Do You Have An Asthma Cough
Asthma cough can be challenging.
It can be embarrassing or awkward to have an ongoing cough, especially amid increased anxiety over health during COVID-19 times.
When we released a blog last year on COVID-19 and asthma coughing, it had a huge response. People with asthma told us about the stigma and social isolation they were feeling about their coughing during the pandemic.
A cough is a way the body attempts to expel irritants in the lungs. But when the cough is due to inflammation of the lungs in asthma, and exposure to triggers, then the cough can continue.
Here is what you need to know about asthma cough.
In asthma, the airways are inflamed and overly responsive to triggers, such as cold and dry air, colds and flu, smoke, dust, and pollens. For some people, the coughing can start after exercise.
The amount and severity of cough can change depending on the weather and the season.
Taking your preventer medication as prescribed, and in line with your , may improve the cough symptoms by reducing the inflammation in the airways.
We encourage you if you are experiencing any asthma symptoms, to speak with your doctor as it may indicate that you are due for an asthma review.
Identifying An Asthma Cough
The purpose of a cough is to remove foreign particles and bacteria to prevent a possible infection. There are two types of coughs: productive and nonproductive. When a cough is productive, it means that a noticeable amount of phlegm expelled. This enables the lungs to get rid of harmful substances.
Coughing in people with asthma can be helpful because its one of the bodys natural defense mechanisms. A productive asthmatic cough will expel phlegm and mucus from the lungs. In most cases of asthma, the cough is considered nonproductive. A nonproductive cough is a dry cough. Its a response to an irritant that forces the bronchial tubes to spasm . Swelling and constriction of the airways, which prompts this type of nonproductive cough, characterize asthma.
An asthma cough is also often accompanied by wheezing. This is a high-pitched whistling sound caused by a constricted airway.
What Are The Symptoms Of A Cough And Nausea
Cough, Decreased appetite, Nausea or vomiting and Thick saliva or mucus. WebMD Symptom Checker helps you find the most common medical conditions indicated by the symptoms cough, decreased appetite, nausea or vomiting and thick saliva or mucus including Bronchitis, Asthma , and Food poisoning.
Recent Posts
You May Like: Does Ibuprofen Make Asthma Worse
Can You Have Asthma And Bronchitis At The Same Time
People with asthma can also have acute bronchitis. They may notice their asthma symptoms become worse as a consequence. They may experience:
- shortness of breath
- wheezing
- pain and discomfort when breathing
Sometimes, people with severe bronchitis and asthma may have to go to the hospital because mucus has clogged the airways into their lungs so much.
How Do I Know If Its Smokers Cough
Smoking is also a major cause of persistent cough, which usually affects long-term smokers.
The toxins in the cigarette damage the airways resulting in a smokers cough. Prolonged coughing can cause hoarseness and chest pain which further leads to lung cancer.
A smokers cough is more like a forceful cough during which a person pushes out air to clear the irritants blocking the airways.
Common symptoms of smokers cough include:
- Last longer than 2-3 weeks.
- Wheezing or crackling sound.
- The cough produces phlegm and mucus.
- Worse coughing when you wake up in the morning.
You May Like: How To Get Rid Of Asthma Without Inhaler
When To See A Gp
Most cases of acute bronchitis can be easily treated at home with rest, non-steroidal anti-inflammatory drugs and plenty of fluids.
You only need to see a GP if your symptoms are severe or unusual.
For example, see a GP if:
- your cough is severe or lasts longer than 3 weeks
- you have a high temperature for more than 3 days this may be a sign of flu or a more serious condition, such as pneumonia
- you cough up mucus streaked with blood
- you have an underlying heart or lung condition, such as asthma, heart failure or emphysema
- you’re becoming more breathless
- you have had repeated episodes of bronchitis
A GP may need to rule out other lung infections, such as pneumonia, which has symptoms similar to those of bronchitis.
If they think you may have pneumonia, you’ll probably need a chest X-ray and a sample of mucus may be taken for testing.
If a GP thinks you might have an underlying condition, they may also suggest that you have a lung function test.
You’ll be asked to take a deep breath and blow into a device called a spirometer, which measures the volume of air in your lungs.
Who Can Get Asthma
Anyone can develop asthma at any age. People with allergies or people exposed to tobacco smoke and secondhand smoke are more likely to develop asthma.
Statistics show women tend to have asthma more than men, and asthma affects Black Americans more frequently than other races.
When a child develops asthma, healthcare providers call it childhood asthma. If it develops later in life, its adult-onset asthma.
Children do not outgrow asthma. They may have fewer symptoms as they get older, but they could still have an asthma attack. Your childs healthcare provider can help you understand the risks.
Also Check: Does Allergy Cause Asthma
History And Physical Examination
Your physical examination will include checking your vital signs, such as your temperature, pulse, and breathing rate. A fever can be an indication of an infection. Rapid breathing or a rapid heart rate can be a sign of a severe infection or an impending asthma attack.
Your doctor will listen to your breathing sounds with a stethoscope, which will help determine whether your congestion is on one side of the lungs or both.
- Generally, with asthma and allergies, congestion affects both lungs.
- Congestion can be limited to one lung or one section of a lung when there is another cause, such as an infection.
Charcoal Or Gray Phlegm
We tend to see charcoal or sooty looking phlegm in people who work in coal mines and factories or are really heavy smokers.
If you work in a factory where theres a ton of smoke and dont wear a mask, youre inhaling all that in and its causing an inflammatory reaction in your airways that produces phlegm. The irritants are mixed in with the phlegm and when you cough, it comes out.
Coughing up blood with asthma underlines that some medical problem is happening in the lungs / respiratory system. Coughing up blood is not due to the presence of an asthma condition because asthma alone does not cause one to have mucus or bloody sputum. The cough with blood originates from the upper respiratory tract, such as from sinuses or nasopharynx, though it is not always easy to detect the source of blood.
Nevertheless, the condition should be taken seriously and diagnosed to determine what the person is suffering from. In medical knowledge, there are several causes for which coughing up blood can happen such as gingivitis, bleeding gums, blood clot in the lung, bronchitis, cystic fibrosis, bronchiectasis, throat irritation due to violent coughing, nosebleed, laryngitis, lung cancer, Goodpastureâs syndrome, pneumonia, necrotic pneumonia, lung injury, lung trauma, parasitic lung infection, anaerobic pneumonia, Serratia marcescens lung infection, pulmonary aspiration, pulmonary edema, tuberculosis, Wegenerâs granulomatosis and systemic lupus erythematosus.
Don’t Miss: Does Weight Gain Make Asthma Worse
My Child Coughs A Lot Could It Be Asthma
Cough is quite a common symptom along with wheezing in babies and young children when they have colds and viruses. If your child coughs a lot, it could be worth getting them checked out by a medical professional.
Asthma is more likely be the cause of the cough is dry if the cough or wheeze wont go away or keeps coming back, occurs more at night or early in the morning, they have symptoms after running around, laughing or being in the cold, wheeze without other cold symptoms, and there are other symptoms such as breathlessness,
Monitor when your child has a cough so you can tell your doctor and determine potential triggers.
Why Do Children Have Mucus In Their Vomit
When young children have chest congestion, theyre are not good at blowing their nose or coughing out the phlegm stuck in their throat.
This means all the excess mucus is being swallowed. With so much mucus finding its way to the stomach, the child suffers from an upset stomach or vomiting after intense coughing, and there will be mucus in the vomit.
Recommended Reading: How To Make A Homemade Inhaler For Asthma
Signs You Actually Have Severe Asthma
Breathing is just one of those things you take for granted until it feels like every inhale or exhale is a struggle. Unfortunately, people with severe asthma have to deal with breathing issues way more often than anyone should, and it can be completely terrifying.
Asthma is a respiratory condition that affects the airways that extend from your nose and mouth to your lungs, according to the National Heart, Lung, and Blood Institute . When youre exposed to triggers like animal fur, pollen, mold, exercise, and respiratory infections, these airways can narrow, restricting your airflow. This can then make the muscles surrounding your airways constrict, making it even harder to breathe, and cause your airways to produce more mucus than normal, further compounding the problem. All together, this can lead to asthma symptoms like shortness of breath, coughing, wheezing , and chest tightness or pain, according to the NHLBI.
Like most health conditions, asthma severity runs along a spectrum, Emily Pennington, M.D., a pulmonologist at the Cleveland Clinic, tells SELF. Some people have cases where they experience minor symptoms here and there . Others can have asthma that is basically an ever-present problem and might result in scary asthma attacks, which is when symptoms ramp up in severity and can even become life-threatening.
Related:
How To Stop Asthma Cough

This article was co-authored by Shaun Berger, MD. Dr. Shaun Berger is a board certified Pediatrician based in the San Diego, California metro area. Dr. Berger provides comprehensive primary care for newborns, children, and adolescents, focusing on preventive medicine. Dr. Berger earned a BA in Psychology from the University of California, San Diego and an MD from the University of Illinois at Chicago. Dr. Berger then completed a residency at the UCSF/Fresno Community Medical Centers/Valley Childrens Hospital where he was elected Chief Resident. He has been awarded the UCSF Foundation Award and is a Fellow of the American Academy of Pediatrics.There are 16 references cited in this article, which can be found at the bottom of the page.wikiHow marks an article as reader-approved once it receives enough positive feedback. In this case, 100% of readers who voted found the article helpful, earning it our reader-approved status. This article has been viewed 76,283 times.
Many people are familiar with common asthma symptoms like tightness in the chest and difficulty breathing. Coughing is another troublesome symptom of asthma, the inflammatory lung disease which narrows the breathing airways. To stop an asthma-related cough, identify and avoid your triggers, take medication to treat your asthma, and make yourself comfortable.
You May Like: Asthma Remedies Without Inhaler
Serious Symptoms That Might Indicate A Life
In some cases, coughing up blood can occur with other symptoms that might indicate a serious or life-threatening condition that needs evaluation in an emergency setting. Seek immediate medical care if you, or someone you are with, have any of these life-threatening symptoms:
-
Bloody stools or urine
Recommended Reading: How To Get Rid Of Asthma Without Inhaler
Southern Cross Medical Library
The purpose of the Southern Cross Medical Library is to provide information of a general nature to help you better understand certain medical conditions. Always seek specific medical advice for treatment appropriate to you. This information is not intended to relate specifically to insurance or healthcare services provided by Southern Cross. For more articles go to the Medical Library index page.
Read Also: No Inhaler What Can I Do
Mucus Postnasal Drainage & Cough
The membranes that line your nose, throat and bronchial tubes are very sensitive. Normally, they secrete up to two liters of mucus a day to moisten and protect themselves. When these membranes become irritated, congested, and swollen, they secrete an extra amount of mucus. This mucus helps to protect the lungs and nose from irritating particles and infection.
If you have asthma, your membranes are more sensitive to irritants, such as smoke, cold air, strong odors and dust, causing them to secrete more mucus than normal. Infections may cause even more congestion, mucus, and discomfort. However, increased mucus or yellow mucus does not always mean that an infection is present. Check with your physician if you have more mucus than usual or if it is green or yellow-colored.
Surprising Signs Of Adult
This post is available in: Spanish
That persistent cough that keeps you up at night may stem from more than just a tickle in the back of your throat. It could be adult-onset asthma.
Many people experience a jolt of disbelief when they are diagnosed with asthma later in life, especially if they have never experienced symptoms before. Asthma? That condition that causes kids to wheeze?
It turns out adult-onset asthma is far more common than many people realize. Asthma is often considered a disease of children, so adults may be surprised when they are diagnosed with asthma, says pulmonologist Javier Pérez-Fernández, M.D., the critical care director at Baptist Hospital of Miami.
The number of people with asthma grows every year. Currently, more than 26 million Americans have asthma, according to the U.S. Centers for Disease Control and Prevention. Of those cases, more than 20 million are among adults, with the greatest number of cases among ages 35 and 65.
Asthma is a chronic inflammation of the lung airways that can lead to coughing, chest tightness, shortness of breath or wheezing. Among adults who develop asthma later in life, the symptoms may initially be more subtle than in children, which can cause patients to overlook or ignore the condition. But its important to treat symptoms as soon as possible so they dont become severe, said Dr. Pérez-Fernández, who also serves as director of pulmonology for West Kendall Baptist Hospital.
Read Also: How To Get Rid Of Asthma Without Inhaler
How Can You Tell The Difference Between Covid
Cold and flu season is here, and the new coronavirus that causes COVID-19 is still spreading. With every cough or sniffle, you may wonder if its asthma or allergies, the flu, the common cold or even COVID-19. But how can you tell the difference?
The Asthma and Allergy Foundation of America has created a respiratory symptoms chart to help you recognize the difference between these conditions.
How Mucus Does Its Job
The airways of the lung constantly make mucus. The cells that line the airways have small hairs called cilia.
The cilia rhythmically beat back and forth, sweeping mucus up out of the airways and into the mouth. The mucus takes with it any foreign particles, like dirt, dust, or bacteria. This keeps the airways clean and free from infection.
You May Like: Can Cold Weather Affect Asthma
Brown Or Black Tinged Phlegm
If you have brown or black tinged phlegm it’s likely that this is down to smoking.
Barbara said that this can also occur in people who have COPD , who also suffer with asthma.
She added: “When you stop smoking even just after three days your airways will get less inflamed and you will have less asthma symptoms”.
Asthma UK states: “Coughing up brown phlegm can also be a symptom of pneumonia.
“If youre coughing up brown or black phlegm, it’s really important that you book an appointment with your GP.”
Personal Asthma Action Plan
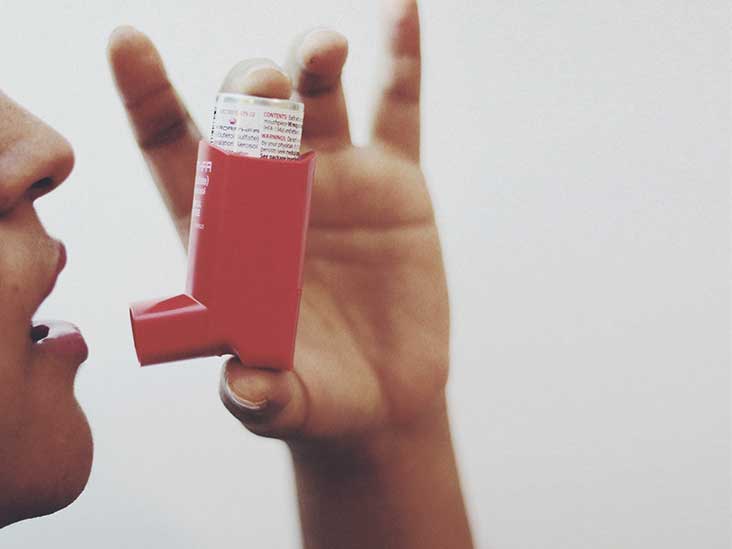
As part of your initial assessment, you should be encouraged to draw up a personal asthma action plan with your GP or asthma nurse.
If you’ve been admitted to hospital because of an asthma attack, you should be offered an action plan before you go home.
The action plan should include information about your asthma medicines, and will help you recognise when your symptoms are getting worse and what steps to take. You should also be given information about what to do if you have an asthma attack.
Your personal asthma action plan should be reviewed with your GP or asthma nurse at least once a year, or more frequently if your symptoms are severe.
As part of your asthma plan, you may be given a peak flow meter. This will give you another way of monitoring your asthma, rather than relying only on symptoms, so you can recognise deterioration earlier and take appropriate steps.
Want to know more?
Read Also: Can Allergies Cause Asthma Attacks
What Does The Colour Of My Phlegm Mean
The colour of your phlegm can change when youre ill.
If you feel unwell and youre worried because your phlegms a different colour or thickness than usual, speak to your doctor. They might look at or test a sample of your phlegm to find out more.
Everyones phlegm looks different and it isnt a completely accurate guide to whats going on in your body. But here’s a general guide to what different colours of phlegm mean:
White phlegm
A bit of white or clear phlegm every now and then is completely normal.
However, if youre producing lots ofwhite or clear phlegm, it could be a sign that your airways are inflamed and your asthma symptoms might be getting worse.
Its worth remembering that your airways include the nose and sinuses, as well as your throat. It may be that the mucus youre coughing up has moved from your nose or sinuses to the back of your throat or chest. If you get symptoms in your nose and sinuses such as mucus, sneezing or an itchy or blocked nose speak to your GP or pharmacist about how you can treat this. Treating your nose and sinuses can improve your asthma symptoms too.
Your preventer inhaler is the number one way to deal with this, as long as youre taking it as prescribed by your doctor or nurse.
If youve been taking your preventer but nothings improving, see your doctor or asthma nurse. They might need to change your medication or help you manage your triggers or allergies, like hay fever.
Yellow or green phlegm
Streaked red phlegm
