Management Of Acute Asthma Exacerbations
SUSAN M. POLLART, MD, MS; REBEKAH M. COMPTON, MSN, FNP-C; and KURTIS S. ELWARD, MD, MPH, University of Virginia Health System, Charlottesville, Virginia
Am Fam Physician. 2011 Jul 1;84:40-47.
Patient information: See related handout on how to treat an asthma attack, written by the authors of this article.
In 2005, the prevalence of asthma in the United States was nearly 8 percent , and approximately 4 percent of Americans experienced an asthma attack., There have been many advances in medical therapy to prevent the worsening of asthma symptoms, including an improved understanding of asthma etiology, identification of risk factors for asthma exacerbations, and evidence supporting the benefits of written asthma action plans.
In persons older than two years with asthma, neither the injectable nor the intranasal influenza vaccine increases the likelihood of an asthma exacerbation in the period immediately following vaccination. However, one study of infants found an increase in wheezing and hospital admissions after intranasal influenza vaccination. Seasonal influenza vaccine does not reduce the risk of developing an asthma exacerbation. Influenza vaccination appears to improve asthma-related quality-of-life in children during influenza season.
Monitoring Asthma At Home
Some people use a handheld peak flow meter to evaluate their breathing and determine when they need intervention, before their symptoms become severe. People who experience frequent, severe asthma attacks should know how to reach help quickly.
Peak expiratory flow can be measured using a small handheld device called a peak flow meter. This test can be used at home to monitor the severity of asthma. Usually, peak flow rates are lowest between 4 AM and 6 AM and highest at 4 PM. However, more than a 30% difference in rates at these times is considered evidence of moderate to severe asthma. People with moderate to severe asthma, particularly those who need daily treatment to control symptoms, often use a peak flow meter to take measurements and compare them to their personal best to help identify signs of worsening asthma or the onset of an asthma attack.
All people with asthma should have a written treatment action plan that was devised in collaboration with their doctor. Such a plan allows them to take control of their own treatment and has been shown to decrease the number of times people need to seek care for asthma in the emergency department.
How Is Hypoxia And/or Hypoxemia Diagnosed Chart
In general, an individual patients hypoxemia is usually diagnosed by oxygen monitors placed on fingers or ears and/or by determining the oxygen level in a blood gas sample . Normal readings are about 95% to 100% oxygen saturation levels; generally, oxygen is supplied if the level is about 92% or below.
Blood Oxygen Levels Chart Using a Pulse Oximetry
| Condition |
The treatment for hypoxia and/or hypoxemia is to give additional oxygen to the patient and into the body as quickly as possible, especially if cerebral hypoxia is suspected, or to treat the underlying cause of the hypoxia.
Many patients will respond to additional oxygen supplied by a nasal cannula. The quicker the oxygen level reaches normal, the better the prognosis is for the patient. However, the timing is very important, because cerebral hypoxia can occur within a few minutes and, in many patients, may not be reversible.
Some patients may be treated in a hyperbaric chamber that increases oxygen concentrations in the blood , while others may require mechanical ventilation with oxygen supplied at higher than normal atmospheric concentrations.
Others, such as mountain climbers or airline passengers, may need only additional oxygen provided by oxygen masks until they reach lower levels where oxygen concentrations are closer to the normal levels in the atmosphere.
However, care must be used when giving oxygen, as it can be toxic to tissues if it is used excessively . Hyperoxia may cause:
How Does Heart Failure Affect Oxygen Saturation
Oxygen saturation is a term used to define how much oxygen the hemoglobin in your blood is carrying. It is commonly measured by a pulse oximetry monitor, a non-invasive device that attaches to the end of your finger. When people with stable COPD also have heart failure, it is not unusual for them to experience shortness of breath, yet have a normal oxygen level reading. In fact, people with both COPD and heart failure could have an oxygen level 96, which would normally be considered high oxygen levels for a COPD patient, and still experience shortness of breath. This is because, as the volume of blood pumped by the heart lessens, the oxygen saturation level is not immediately affected. However, the lower volume of blood being pumped means that your organs are getting less oxygen. Over time, lack of oxygen affects every organ in the body including the lungs, which may eventually lower oxygen saturation./1
Care Advice For Asthma Attack
Evaluating Shortness Of Breath
Depending on your symptoms, your doctor may evaluate your shortness of breath by using pulse oximetry to estimate the amount of oxygen in your blood, an EKG, a chest x-ray, blood work, or pulmonary function tests.
Its important to note that while you may suffer from COPD or asthma, your symptoms can still be managed and allow you to lead a normal life with the right health care team working with you.
Myth 3: I Do Not Need To Take My Inhalers When I Feel Okay
The National Heart, Lung, and Blood Institute strongly recommends taking your long-term control medications each day.1 Asthma is a chronic inflammatory disease. This means that even when you do not have any asthma symptoms, your airways are still inflamed. Long-term control medications reduce the inflammation. With less inflammation, your airways become less sensitive. This prevents symptoms from flaring up, improves your lung function, and reduces the risk of complications.1
It can be hard to remember or want to take your medication when you are feeling fine. Work with your health care provider to find the lowest dose you need to control your symptoms. Make taking your medication part of your daily routine, for example, before you brush your teeth in the morning or when you sit down to eat breakfast. Store your medication in the same place every time. One study showed that people were more likely to take their inhaler if it was stored in the bathroom instead of next to the bed.7
What Is Oxygen Therapy
Oxygen therapy is sometimes simply known as O2 therapy, and it is a fairly common and effective medical treatment that is used to help treat patients dealing with breathing difficulties.
Oxygen is essential for survival, without oxygen, the human body would breakdown and die in a matter of minutes. The air that we breathe every day, the same air that we are breathing right now, contains 21% oxygen.
Oxygen therapy is basically a treatment whereby oxygen is administered at concentrations greater than those found in the air that we breathe.
How Does It Work?
Oxygen therapy works by increasing the amount of oxygen in the blood, helping to combat low blood oxygen levels.
When you undergo oxygen therapy, the oxygen will need to be prescribed to you by a doctor.
A test will be carried out by your doctor to determine how much oxygen you require each minute, and then it will come down to how much you need.
Normally it will be prescribed to you in the form of a standard oxygen concentrator, which is a machine equipped with a motor that can be battery-powered, or mains fed.
It takes in air and filters out the other gases, leaving just the oxygen, which the patient will breathe in via a face mask or a nasal cannula.
These also come in smaller portable sizes for when you have to leave the home.
What Is Intensive Care
The intensive care unit is a specialist hospital ward for treating people who are the most critically ill. Its sometimes called the critical care unit or intensive therapy unit .
In ICU, the team of doctors and nurses are trained to look after patients who are very unwell. Theres usually one nurse for every one or two patients so they can monitor you closely.
If youre having severe asthma symptoms but dont need one-to-one care, you might go to the high dependency unit instead. Here, each nurse may be looking after two or three patients.
Being admitted to ICU or HDU can feel scary. But youre in the right place to get the best treatment to bring your asthma back under control. And the staff are focused on giving you the best care.
If I Think I Have Covid
If you start having symptoms of COVID-19, call your doctor or your local health department within 24 hours. Many states have various testing options, and your doctor or department of health can tell you what to do.
Many doctors have been offering telehealth . If that is an option, ask your insurance company if telehealth is covered under your plan. And if you have Medicare, you might be able to have a virtual visit with your doctor. The government has expanded the coverage of telehealth services during the COVID-19 crisis.
How Are Blood Oxygen Levels Checked Using A Pulse Oximeter
A pulse oximeter is a small, mobile, and handy medical device. It is most commonly used when doctors want to know your blood oxygen levels quickly. It is also used to monitor the response of your body to certain medications or supplemental oxygen. Blood oxygen levels are indicated as SpO2, which is the percent saturation of oxygen in the blood.
The test that measures blood oxygen levels using a pulse oximeter is known as pulse oximetry. The procedure is very simple and requires only clipping the pulse oximeter in between any of the fingers for a few seconds. The reading appears on the pulse oximeter screen. This test may be slightly less accurate than ABG but is easier to perform than ABG tests when needed quickly.
- The brain gets affected when the SpO2 level falls below 80-85%.
- Cyanosis develops when the SpO2 level drops below 67%.
- The normal oxygen levels in a pulse oximeter usually range from 95% to 100%. Note: Normal levels may vary if you have lung disorders. Your doctor can tell what levels are normal for you.
Blood Oxygen Levels Chart Using a Pulse Oximetry
| Condition |
|---|
Exercise: The Key To Breathlessness
The answer to breathlessness from COPD, heart failure and/or skeletal muscle dysfunction is exercise in order to maintain high oxygen levels. In fact, the American College of Cardiology reports that people who have COPD and heart failure together are prime candidates for exercise training.Moreover, skeletal muscle abnormalities can be completely reversed by participating in an exercise training program or a cardiopulmonary rehabilitation program.3
Talk to your health care provider for more information about enrolling in cardiopulmonary rehab. If you are ready to start an exercise program on your own, we recommend reading 11 Tips for Exercising with a Chronic Health Condition.
The Normal Respiratory System
To understand what happens in asthma you need to be familiar with the normal breathing system and how the lungs and airways are arranged.
Normally, air entering through the mouth and nose travels through the main airway through a series of smaller branching airways called bronchi. The bronchi divide up into even smaller airways called bronchioles, which end in millions of tiny air sacs called alveoli.
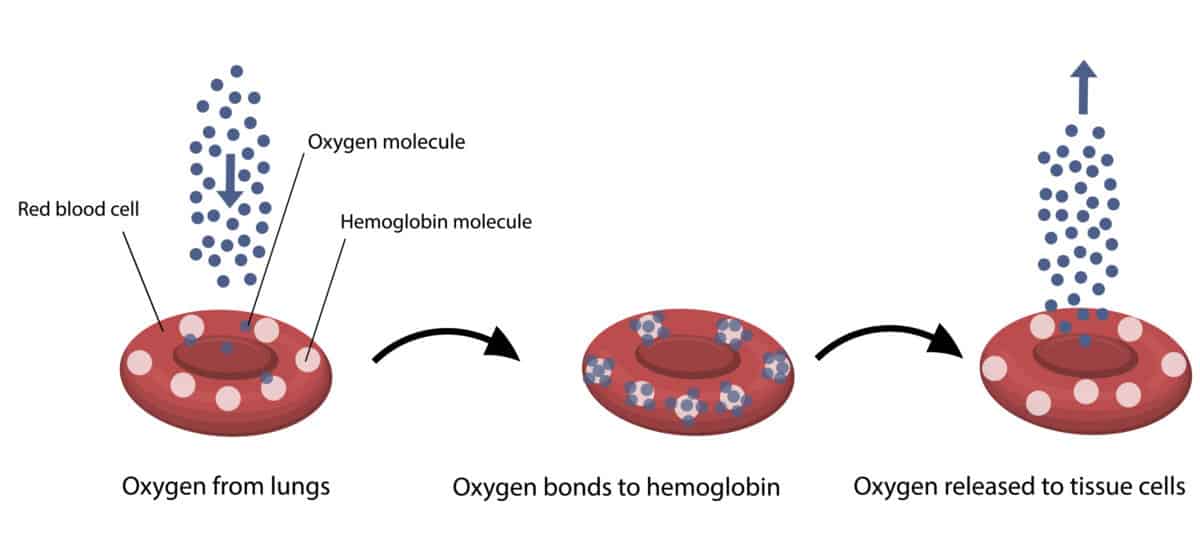
When air enters the alveoli, the oxygen it contains passes through the thin membrane covering each sac into surrounding blood vessels. The oxygen attaches itself to red blood cells which then circulate around the body, releasing the oxygen into the body tissues.
What happens during an asthma attack?
Reactive Airways Dysfunction Syndrome
Reactive airways dysfunction syndrome is a rapid onset and persistent asthma-like disorder that occurs in people with no history of asthma. It is a form of environmental lung disease caused by a single large exposure to nitrogen oxide or volatile organic compounds . People have symptoms similar to those of asthma, including cough, wheezing, and shortness of breath. Treatment is similar to usual treatment for asthma.
Who Is At Risk For Severe Illness From Covid
Many studies to date show no increased risk of COVID-19 infection or severity of COVID-19 disease in people with asthma.3,4,5 A study published in âThe Journal of Allergy and Clinical Immunology: In Practiceâ found that people with well-controlled asthma have less severe COVID-19 outcomes than those with uncontrolled asthma.6 Now is the time to talk with your doctor to make sure your asthma is well-controlled.
The CDC continues to list moderate-to-severe asthma as a chronic lung disease that can make you more likely to have severe illness from COVID-19.
Based on existing evidence, the following adults can be more likely to get severely ill from COVID-19:
- Older adults
- People who are affected by long-standing systemic health and social inequities including:
- People who are Black, Hispanic/Latino, or American Indian/Indigenous American
- People with disabilities
- Smoking
- Solid organ or blood stem transplant
- Stroke
- Substance abuse disorders
Children can be infected with the virus that causes COVID-19 and some children develop severe illness. While some children may be at increased risk due to chronic medical conditions, there are no current data that show asthma is a risk factor for severe disease in children, either.
- Quick-relief medicine
- Inhaled corticosteroids
- Allergy shots
If you have any questions about asthma medicines and the coronavirus, talk with your doctor.
Low Oxygen Levels: How Low Is Too Low And Should You Worry
Low oxygen levels will rob you of your eye sight, short term memory, and your energy. Eventually low oxygen levels will weaken your heart muscle.
Heart Failure IS -> Progressive weakening of your heart muscle!
The world is facing an epidemic of heart failure! This ONE health crisis will rob more productive work years from Americans than any other.
Myth 1: Most Children Will Outgrow Asthma
Some children do seem to outgrow their asthma, but many do not.1 It is not possible to predict who will outgrow his or her symptoms. However, severe asthma is more likely to persist than mild asthma. In one study, 64% of children with mild asthma were symptom-free as adults.2 Only 15% of the children with severe asthma outgrew it. Boys are more likely than girls to outgrow their asthma.3
Interestingly, studies have shown that asthma symptoms reappear later in life.3 A study from Arizona showed that nearly two-thirds of people who were newly diagnosed with asthma at age 22 wheezed before the age of three. The families likely thought the children had outgrown their symptoms. However, it seems that adulthood asthma actually has its roots in early childhood.
Myth 4: If Treatment Is Not Working The Patient Must Be Doing Something Wrong
There are many reasons that asthma might not improve, even if you are taking your medication correctly.
One-half to two-thirds of people take their medication correctly.8 Often the people with the most severe asthma are the most compliant, because their survival depends on it. The fact is that response to treatment is variable from person to person and over time.1 If a person has uncontrolled asthma, it may be that:
- More medication is needed.
- A different type of medication is needed.
- Unidentified triggers are causing asthma to flare up.
- Changes to the Asthma Action Plan are needed to help the patient respond appropriately to worsening symptoms.
- The person has other conditions that need to be treated, such as GERD, COPD, obesity, or vocal cord dysfunction.
It is very common for people to use their inhaler incorrectly, which might mean that too little medication gets into the lungs.8 To be sure you are using your inhaler correctly, bring it to each appointment and review proper technique.
Not all people who take their medications incorrectly do so by choice or carelessness. Many find it difficult to afford medications or to find transportation need to get to medical appointments and the pharmacy.9,10 Bothersome side effects and the inconvenience of taking medications can be barriers as well.10 If you are having these problems, talk with your health care provider so that you can work together to find a solution.
When To Contact A Doctor
Asthma can be life threatening for a child, so it is very important that a person seeks medical attention if a child starts to show symptoms of asthma.
A medical professional will then be able to offer advice on the best methods available to manage the condition.
It is also vital that a person seeks immediate medical help if they experience oxygen deprivation. Symptoms of this can include:
How Does The Coronavirus That Causes Covid
The coronavirus spreads through close contact from person to person. A person with the virus can spread it to others by talking, coughing, sneezing, singing, or breathing. The virus will be in droplets that are exhaled from the mouth or nose out into the air. These droplets can vary in size from small to large. Large droplets are heavy and quickly fall to the ground/surface below. Small droplets can linger in the air longer and spread more easily. This is called airborne transmission.
People who are within 6 feet of someone who is ill with COVID-19 may be at greatest risk for becoming infected. But it may be possible to catch the virus even if you are more than 6 feet away from an infected person because very small droplets can linger in the air. If someone who is sick coughs on or near your face, you may get infected. People may be infected with the coronavirus and not show any symptoms. They may spread the virus without knowing it. The virus may also spread through direct contact with a person who has COVID-19.
Even if you are fully vaccinated, the CDC now recommends wearing a face mask in places where itâs hard to keep a 6-foot distance from others to help stop the spread of infection. If you aren’t wearing a face mask, cough/sneeze into your elbow or a tissue. If you use a tissue, throw it away. In either case, wash your hands after you cough or sneeze.
Chronic Obstructive Pulmonary Disease

COPD is a lifestyle related lung diseases characterized by progressive loss of lung function and gas exchange abnormality. The major sites of airflow obstruction in COPD is the small airways . Alveolar walls maintain patency of the small airway by exerting radial traction by the elastic fibers. Alveolar wall destruction leads to loss of these elastic fibers, resulting in airflow obstruction. Alveolar wall destruction also causes loss of the alveolar surface area and pulmonary capillaries, resulting in gas exchange abnormalities. Other mechanisms of airflow obstruction include bronchial mucosal inflammation, edema or fibrosis, and mucus hypersecretion. The most common gas exchange abnormalities in COPD patients include arterial hypoxemia, with or without hypercapnia. The major mechanism of hypoxemia in COPD is V/Q mismatch. Gas exchange abnormality depends on the phenotype of COPD. Phenotyping in COPD is not new as Burrows distinguished the two phenotypes of COPD as early as 1963. He proposed the following classification of COPD based on clinical, roentgenologic, and physiologic characteristics: Type A , Type B , or type X . Type A patients show hyperinflation decreased elastic recoil of the lung, mild hypoxemia and rarely hypercapnia, whereas, Type B patients develop worse hypoxemia and hypercapnia. They also develop cor pulmonale more frequently.
Being Discharged From Hospital After Being In Icu
Once youre well enough, youll be discharged from hospital and can go home.
You should be referred to a specialist consultant or a specialist asthma care centre for a follow-up appointment to help you manage your asthma going forward. Find out what to expect from specialist asthma care.
Before you leave hospital make sure:
- you have a to take away with you
- you see someone in the specialist respiratory team to review your treatment plan and explain anything you need to know
- you understand any medicines you need to take and how to use them, and have collected them from the hospital pharmacy
- the hospital has told your GP about your asthma attack and you have a follow-up appointment booked as soon as possible, and certainly within two days of leaving hospital
- you know when youll need a follow-up with a specialist consultant or at an asthma care centre
How Is Pulse Oximetry Used To Determine The Severity Of Acute Asthma In Children
In children, pulse oximetry is often used to grade severity of acute asthma. Oxygen saturation of 97% or above constitutes mild asthma, 92-97% constitutes moderate asthma, and less than 92% signifies severe asthma. Although an isolated pulse oximetry reading at triage is not predictive in most cases , serial monitoring of pulse oximetry status can provide more subtle evidence for or against the need for hospital admission.
Diagnosing Asthma In Older People
Older people are more likely to have other lung diseases that also cause shortness of breath , so doctors have to determine how much of the person’s breathing difficulty is related to asthma and reversible with the appropriate anti-asthma therapy. Often, in these people diagnosis involves a brief trial of drugs that are used to treat asthma to see whether the person’s condition improves.
When To See A Doctor
If you or a family member is experiencing a first onset of symptoms of asthma, see your doctor. They may then refer you to a specialist. You should also see your doctor when you are experiencing less serious symptoms, and the tools you have to improve the asthma are not working.
When you seek medical attention for asthma your doctor can classify the severity of your asthma and select the best treatment. Because the degree of your asthma may change over time, its important to see a doctor regularly to adjust your treatment accordingly.
If you think you or a family member is experiencing an asthma attack, call 911 or local emergency services, or go to your nearest emergency room.
When To Call A Professional
- Wheezing
- Difficulty breathing
- Cough
Some children with asthma may not complain specifically of shortness of breath. However, they may flare their nostrils or use their chest and neck muscles when breathing. These are signs that they are having trouble.
If you already have been diagnosed with asthma, call your doctor if your symptoms:
- Are getting worse
- Are not being controlled by your regular medications
For example, call your doctor if you must use your rescue bronchodilator more than four times a day. Also call if your peak-flow-meter readings are in the yellow or red zones.
If you have an asthma attack and your symptoms persist despite your usual medications, seek emergency help immediately.
