Differences Between Copd And Asthma
There are a number of other differences between COPD and asthma as well.
-
Often diagnosed during childhood or adolescence
-
Symptoms more likely to occur episodically and/or at night
-
Commonly triggered by allergens, cold air, exercise
-
People who have asthma are more commonly nonsmokers
-
Comorbid conditions include eczema and allergic rhinitis
-
Treatment usually involves inhaled steroids
-
Airflow restriction mostly reversible
-
Likely to cause morning cough, increased sputum, and persistent symptoms
-
Exacerbations commonly triggered by pneumonia and flu or pollutants
-
Most people who have COPD have smoked or had significant secondhand smoke exposure
-
Comorbid conditions include coronary heart disease or osteoporosis
-
Treatment usually involves pulmonary rehabilitation
-
Airflow restriction is permanent or only partially reversible
Once you develop COPD, your symptoms will generally be chronic. Over time, with COPD, you are likely to experience symptoms that are not typical for asthmalosing weight, decreased strength, and diminished endurance, functional capacity, and quality of life.
Vaccine Distribution In Canada
As part of the Canadian Thoracic Societys COVID-19 Respiratory Roundtable panel representing Canadians living with lung disease, Asthma Canada signed a joint statement titled Prioritization of Canadians with Lung Disease in COVID-19 Vaccination Rollout. Alongside other lung health organizations, Asthma Canada is urging federal, provincial and territorial governments to prioritize people living with lung disease who are at higher risk for more serious COVID-19 complications in the vaccination rollout. From Canadians living with a lung disease such as asthma, chronic obstructive pulmonary disease , cystic fibrosis, lung cancer, pulmonary fibrosis, pulmonary hypertension, and pre- and post-lung transplant, there is widespread concern regarding when in the vaccine rollout in the provinces and territories they will have the opportunity to receive the vaccine.
We will continue to advocate for our community on this subject and will share more information as it becomes available.
Read the full statement here:English | French
Are Asthma And Copd Disabilities
According to the Asthma and Allergy Foundation of America , the American Disabilities Act and Section 504 state that having a mental or physical impairment that severely limits one or more life activities, including breathing, can be considered a disability.
For people with asthma, this applies even if symptoms only show at certain times, and if the person uses medication, such as an inhaler, to control the problem.
To qualify for social security disability benefits with COPD, a person must have:
- A forced expiratory volume one that is the minimum for your height or less, from 1.05 to a person who is 5 feet tall to 1.65 to someone who is 6 feet tall.
- Chronic impairment of gas exchange resulting from a documented COPD.
Those who do not meet these requirements may be able to get other types of help, such as as medical-vocational allowance for people on a low income.
Read Also: Treat Asthma Cough
Asthma And Copd May Require Multiple Treatments
Dear Mayo Clinic:
I am an active 84-year-old man and was diagnosed with asthma and COPD a few years ago. My pulmonologist prescribed two medications Advair and Spiriva that seem to do the same thing. Why would I need both medications and are there other options?
Answer:
The medications you mention include three drugs because Advair contains two different medications. Spiriva is approved for treating chronic obstructive pulmonary disease . Advair is approved for both asthma and COPD. For people with moderate to severe COPD, research has shown a number of benefits with triple therapy like yours.
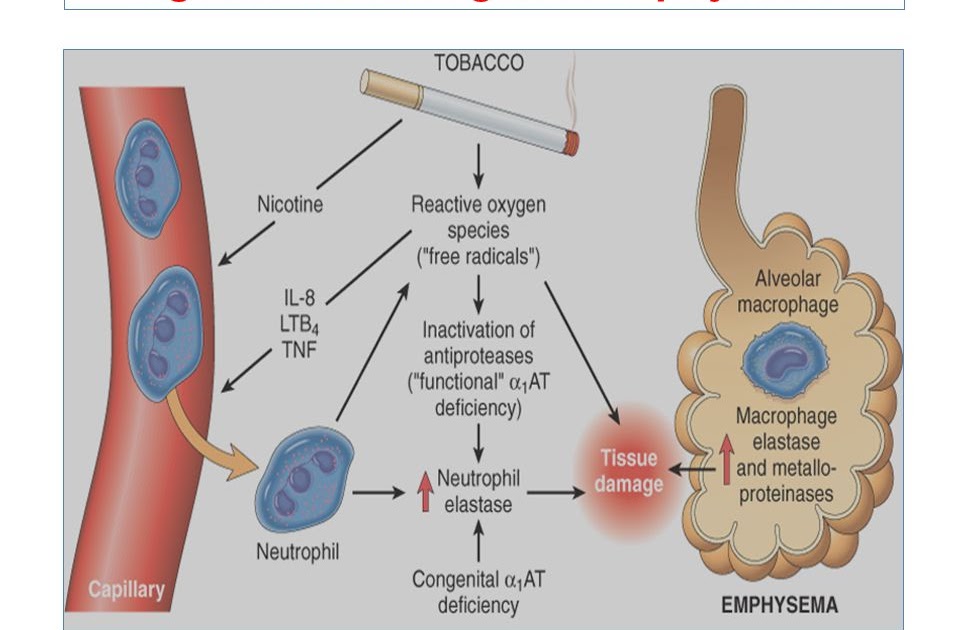
COPD is a lung disease that blocks airflow and makes breathing difficult. In most cases, the lung damage that leads to COPD is caused by cigarette smoking. But other irritants can cause COPD, too, including cigar or pipe smoke, air pollution and certain occupational exposures. In some cases, COPD results from a genetic disorder that causes low levels of a protective protein called alpha-1-antitrypsin.
Asthma occurs when the airways in the lungs become inflamed and constricted. This may be triggered by allergies or viral infections. During an asthma attack, the airways thicken due to inflammation, the muscles of the bronchial walls tighten, and the airways produce extra mucus that increases obstruction.
Paul D. Scanlon, M.D., Pulmonary and Critical Care Medicine, Mayo Clinic, Rochester, Minn.
Q: How Is Acos Treated
Your provider can begin treatment if you have COPD or asthma alone. But if you have ACOS, you may want to see a pulmonologista specialist in lung health. People with ACOS often experience more severe symptoms than those with a single lung disease, but working with a specialist can help you feel better. Treatment for ACOS usually includes medicine.
You May Like: What Happens If You Smoke Weed With Asthma
Is It Asthma Or Copd
Because asthma and COPD look similar, causing symptoms such as coughing, wheezing, and difficulty breathing, it’s often challenging to differentiate between the two illnesses, especially when they co-occur. Yet there are some subtle differences. For instance, asthma episodes often occur at night and after exposure to allergens, while people with COPD commonly experience coughing and mucus in the mornings, along with chest symptoms that can linger throughout the day. But using symptoms alone may not be enough to accurately identify the conditions and determine how best to treat them.
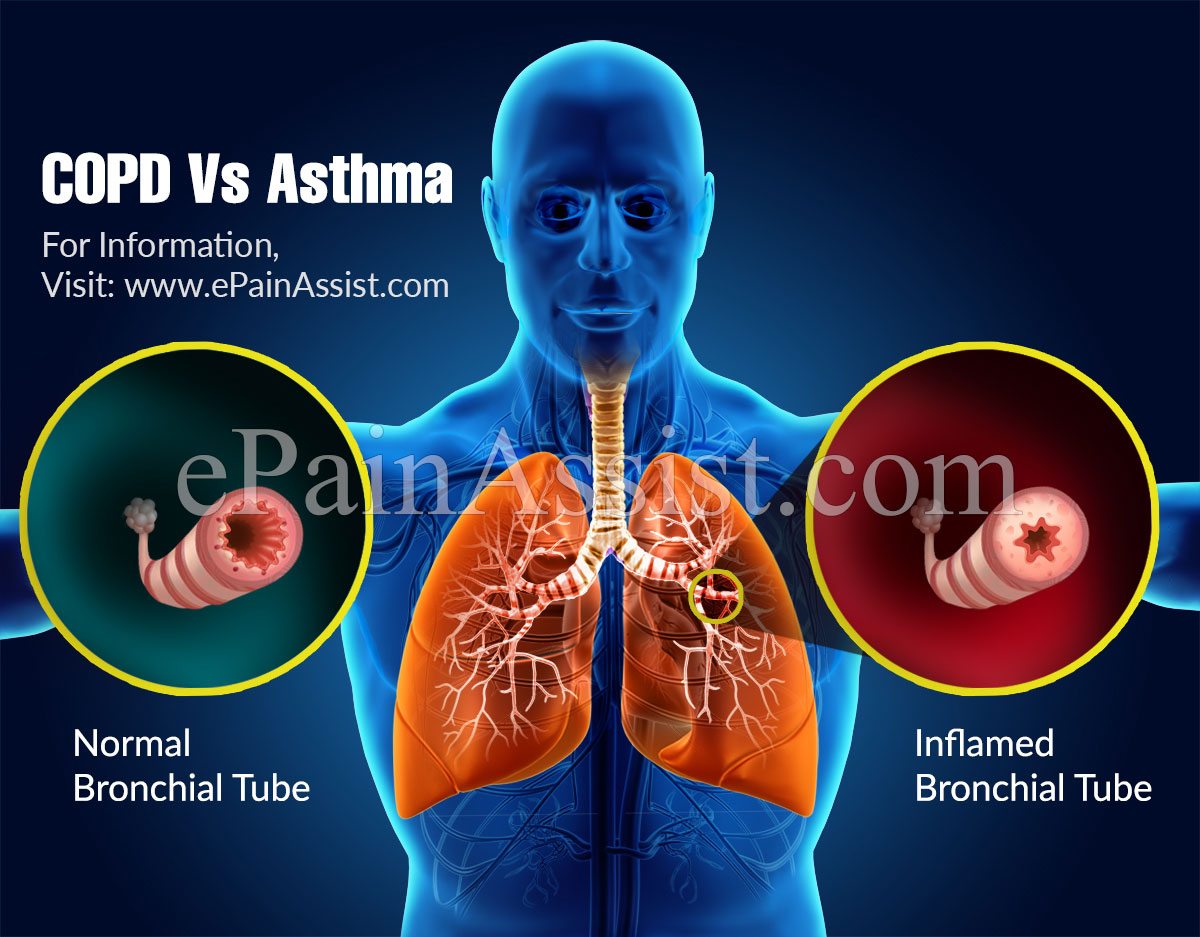
Asthma Vs Copd: What’s The Difference
It is no surprise that asthma and chronic obstructive pulmonary disease are often mistaken for one another they are both conditions that affect the lungs and make breathing more difficult. Despite their many similarities, asthma and COPD are not the same. In honor of November being National COPD Awareness Month, it is time to finally clear up the question of whether asthma and COPD are the same thing.
Below, we will look at the definitions of the two diseases, along with the symptoms, causes and treatments for each. We will also discuss when to see a medical professional for lung damage to help raise COPD awareness this month.
Don’t Miss: Asmanex Weight Gain
Similarities And Differences In Regular Standard Treatment Of Asthma And Copd
-
In both diseases the adequate treatment may reduce symptoms and number of exacerbations and improve the quality of life.
-
Treatment of asthma is characterized by suppression of inflammation.
-
Treatment of COPD is characterized by decreasing of symptoms.
The GOAL of treatment in ASTHMA is to: reduce inflammation and to achieve¸total control . The GOAL of treatment in COPD is to: reduce symptoms, prevent exacerbations and decrease mortality . In both asthma and COPD almost the same drugs are used, but not in the same order and the same efficiency in treatment.
Prevalence Of The Asthma
It is well known that some patients suffer from both asthma and COPD, and that they represent an important clinical population with peculiar characteristics. , In fact, it has been frequently observed that some patients with asthma have an accelerated decline in lung function, especially if they are smokers, , and that some patients with COPD have a good response to treatment with bronchodilators and ICS. It is still an open question whether the overlap syndrome represents the coexistence of two distinct airway diseases or whether there are common underlying pathogenic mechanisms leading to this phenotype. In comparison to previous studies that have considered selected groups of patients, such as COPD patients, , our study enabled us to assess the prevalence of the asthma-COPD overlap syndrome in the general population. We found that this prevalence ranged from a minimum of 1.6% in the 2044 age group to 4.5% in the 6084 age group.
Don’t Miss: What Happens If You Smoke Weed With Asthma
Comparing Asthma And Copd
Both asthma and COPD hamper your respiratory system, making breathing uncomfortable, and at times, nearly impossible. Each poses a danger to your lung function, overall health, and quality of life, but the two conditions differ in some important ways, and its important to know how to tell them apart:
Inflammation
Both asthma and COPD involve inflammation of the airways, but that inflammation comes in different ways. In the case of asthma, allergic triggers tend to inflame your airways, and the list of potential allergens is long. From dust to dander, asthmatics know to watch out for particles that will inflame their sensitive system.
In comparison, the inflammation of COPD is always present when chronic bronchitis is involved, but it isnt always the most pronounced symptom. In fact, breathing discomfort is generally due to dead or paralyzed tissue, not inflamed muscles in the airways. COPD inflammation also doesnt respond well to anti-inflammatory medications .
Persistence
While both conditions are chronic, COPD symptoms are steadier than asthma symptoms. For instance, asthma symptoms or attacks can come on suddenly in the presence of a trigger, but COPD symptoms are always there: patients often wake with a congested chest and a productive cough, and though it may lighten during the course of the day, breathing problems never disappear completely.
Recovery
Q& a: When Youre Diagnosed With Both Asthma And Copd
When youre diagnosed with asthma or chronic obstructive pulmonary disease , it can be difficult to breathe. But did you know that about 15% to 55% of adults with one of these lung diseases actually qualify for a dual diagnosis?
This dual diagnosis is called asthma-COPD overlap syndrome . People at risk for ACOS are typically those with asthma who smoke, but healthcare providers also see cases in those who dont use tobacco. The right diagnosis is important with lung conditions, and education is key to understanding treatment options. To learn more about ACOS, read the answers to some common questions below.
Read Also: How To Treat Asthma Attack Without An Inhaler
Response Rates And Sample Characteristics
The response rate was minimum in the elderly and maximum in people aged 4564 . The distribution of sex and smoking habits showed a statistically significant variation across age groups. The percentage of women was 53.6%, 52.2% and 42.7% in the 2044, 4564 and 6584 yrs age groups, respectively. In these age groups, 26.6%, 23.4% and 9.6% of the subjects were current smokers, while 55.4%, 42.2% and 53.0% of the subjects never smoked.
Screening Questionnaire Respiratory Outcomes And Potential Confounders
The GEIRD Screening Questionnaire is a modified version of questionnaires used in previous international and national studies. . It is aimed at investigating the presence of symptoms of asthma, allergic rhinitis, chronic bronchitis/COPD and dyspnoea, and some environmental exposures. Questions on doctor diagnosis of asthma and COPD were also included.
Based on the answers to the questionnaire, a subject was considered to have a physician diagnosis of:
-
asthma if s/he answered affirmatively to both questions Have you ever had asthma? and Was this confirmed by a doctor?
-
COPD if s/he gave a positive answer to the question: Have you ever been told by a doctor that you have or had chronic bronchitis, chronic obstructive pulmonary disease or emphysema?.
The self reported physician diagnosis of COPD relied on the knowledge of the terms COPD, chronic bronchitis and emphysema. These are the most widely used terms when Italian doctors give patients a diagnosis of COPD.
The questionnaire also collected information on the presence of the following respiratory symptoms/conditions: wheezing or whistling in the chest in the last 12 months, asthma attacks in the last 12 months, current use of medicines for asthma, allergic rhinitis, chronic bronchitis . The dyspnoea scale of Medical Research Council was used as a measure of the functional limitation due to breathlessness .
Also Check: Are Chihuahuas Good For Asthma
Accelerated Decline In Lung Function
Since COPD represents incomplete reversibility of airflow obstruction, then any risk factor that leads to accelerated loss of lung function will contribute to the development of COPD. Several risk factors for accelerated decline in include age, smoking, BHR, asthma and exacerbations or lower respiratory infections. Increasing age is associated with decline in lung function, both in asthma and in those without asthma.
Smoking
Loss of lung function is accelerated by smoking by up to 50 ml per year, and there is an established doseâresponse relationship. The loss of lung function with smoking may even be greater in those with asthma, such that smokers with asthma can develop COPD. Importantly, quitting smoking slows the decline in lung function. In the Lung Health Study, the annual decline in FEV1 in people who quit smoking at the beginning of the 11 year study was 30 ml/year for men and 22 ml/year for women. Continued smoking led to a decline in FEV1 of 66 ml/year in men and 52 ml/year in women.
Bronchial hyper-responsiveness
Asthma
The deficits in lung function in asthma seem to arise early in the course of the disease, and may be an effect of incomplete lung growth. In one study, abnormal lung function at age 26 in patients with asthma was related to male sex, BHR at age 9 years, early onset of asthma and reduced lung function by age 9 years.
Exacerbations
Myth No : There’s No Truly Effective Treatment For Copd
COPD is not curable, but proactive condition management can improve ones ability to function. There are several lifestyle modifications and medical interventions that have been proven to make a difference.
Quitting smoking is the most important change a patient can make. Good nutrition is also important, as is exercise . Patients should also keep vaccinations up to date for pneumococcal pneumonia, influenza and pertussis .
Beyond that, drug therapies such as inhalers, corticosteroids and muscarinic antagonists have also shown improvements for patients. In severe cases, patients may need supplemental oxygen to support blood oxygen levels or may benefit from using a ventilator to assist with breathing, especially while asleep.
Also Check: Diy Inhaler Holder
Inflammatory Mediators Involved In Asthma
Chemokines are important in the recruitment of inflammatory cells into the airways and are mainly expressed in airway epithelial cells . Eotaxin is selective for eosinophils, whereas thymus and activationregulated chemokines and macrophage-derived chemokines recruit Th2 cells . Cysteinyl leukotrienes are potent bronchoconstrictors and proinflammatory mediators mainly derived from mast cells and eosinophils . Cytokines orchestrate the inflammatory response in asthma. Key cytokines include IL-1 and TNF, and GM-CSF. Th2-derived cytokines include IL-5, which is required for eosinophil differentiation and survival IL-4, which is important for Th2 cell differentiation and IL-13, needed for IgE formation . Histamine is released from mast cells and contributes to bronchoconstriction and inflammation . Nitric oxide , a potent vasodilator, is produced from syntheses in airway epithelial cells . Exhaled NO is increasingly being used to monitor the effectiveness of asthma treatment . Prostaglandin D2 is a bronchoconstrictor derived predominantly from mast cells and is involved in Th2 cell recruitment to the airways .
Airway structural cells involved in the pathogenesis of asthma are: airway epithelial cells, airway smooth muscle cells, endothelial cells, fibroblasts and myofibroblasts and airway nerves .
Talking To Your Doctor
Symptoms of asthma and COPD are similar to symptoms of other complications of lupus. This can prevent people from receiving the right treatment. Talk to your doctor about ways to prevent asthma, COPD, and other conditions. A healthy diet and avoiding smoking may reduce your risk. Avoiding certain triggers may also help.9,10
Talk to your doctor if you notice new or worsening respiratory symptoms. Some common symptoms of asthma and COPD include:9,10
- Shortness of breath
- Trouble sleeping because of shortness of breath
- Coughing or wheezing attacks worsened by a respiratory infection
To diagnose asthma or COPD, your doctor will test your lung function. Treatment of asthma usually involves taking medicines and avoiding triggers . The right medicine for you depends on many factors.9,10
Severe asthma attacks can be life-threatening. Talk to your doctor ahead of time about what to do if your symptoms worsen. Ask about when to seek emergency treatment.9
Read Also: Will Losing Weight Help Asthma
It’s Easy To Get The Care You Need
See a Premier Physician Network provider near you.
Chronic obstructive pulmonary disease and asthma are often mistaken for one another. Thats understandable. These two lung diseases share some of the same symptoms: wheezing, chronic coughing and shortness of breath.
To further cloud the distinction, about 40 percent of people who have COPD also have asthma. Asthma and COPD share some of the same risk factors such as smoking tobacco, exposure to air pollutants at home and work, genetics and respiratory infections. And asthma is considered a risk factor that increases the chances of developing COPD.
But asthma and COPD are two distinct diseases. Here are two distinct differences.
- Age at diagnosis: Asthma, in most cases, is diagnosed in childhood. COPD symptoms usually first appear after the age of 40 and, in most cases, among current or former smokers.
- Disease triggers: Asthma is usually triggered by exposure to allergens, cold air and exercise. COPD is primarily aggravated by respiratory tract infections, such as pneumonia and the flu, and exposure to environmental pollutants.
A third difference is that COPD ranks high in third place on the Centers for Disease Control and Preventions list of leading causes of death, after heart disease and cancer.The good news is that with proper treatment, such as quitting smoking, airway-opening medications and avoidance of irritants and allergens, people with asthma and COPD can live more comfortably.
Whos Likely To Have Asthma Copd Or Aco
People who smoke or breathe in pollution or chemicals at work for many years have higher chances of having COPD. That’s why the condition often starts in middle age or later in life.
Asthma is sometimes caused by gene changes that are passed down through families. If one of your parents has the disease, you’re more likely to have it.
Symptoms of asthma often start in childhood, and the condition is one of the most widespread long-term illnesses in kids. It affects about 1 in 10 children.
Besides a family history of the condition, a few things can raise your chances of asthma:
- Smoking
- Being around chemicals or other irritants in the air
People who get ACO tend to be over 40 but younger than people with just COPD, and they have allergies .
Recommended Reading: Asthma Small Airways
