Asthma Allergies And Covid
Throughout the pandemic, having asthma was considered a risk factor for severe COVID-19. But new data show that people with asthma are relatively protected from severe COVID-19, said Geoffrey Chupp, MD, professor of medicine in the Section of Pulmonary, Critical Care & Sleep Medicine at Yale School of Medicine .
We looked at 8,000 hospital admissions of patients with COVID-19, and we found that the patients who were diagnosed with asthma – about 10% of the patients – were more likely to survive compared to those people who didnt have asthma, Chupp said. He emphasized that the patients had asthma, not smoking-related lung diseases such as emphysema and COPD.
Its possible that some of the medications used for asthma helped to reduce the inflammation that COVID-19 causes, Chupp said. Its also likely that the type of immune response most asthmatics have, the allergic response, protected them from severe lung damage, he added.
However, after these patients recovered from COVID-19, their asthma became reactivated. As they healed, their natural immune response came back with more activity, explained Chupp. Were seeing a fair amount of post-COVID uncontrolled asthma. Most people do well but some have this persistence, a kind of long-hauler problem, although most of them will get better with time.
Asthma, Allergies & Pollen
What Should I Do If I Have A Severe Asthma Attack
A severe asthma attack needs immediate medical care. The first step is your rescue inhaler. A rescue inhaler uses fast-acting medicines to open up your airways. Its different than your normal maintenance inhaler, which you use every day. You should only use the rescue inhaler in an emergency.
If your rescue inhaler doesnt help or you dont have it with you, go to the emergency department if you have:
- Anxiety or panic.
- Bluish fingernails, bluish lips or gray or whitish lips or gums .
- Chest pain or pressure.
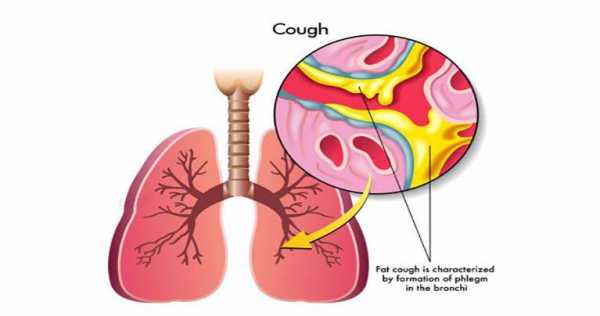
What Is A Cough
A cough is an automatic response to irritation of the airways in the lungs. See the separate leaflet called Cough for more information.
Having a cough is the main symptom of an upper respiratory tract infection . However, a cough can also be a symptom of other conditions such as asthma or other lung diseases.
This leaflet only discusses cough medicines when used to treat coughs caused by an URTI. It assumes you are confident that you know you have not got anything more serious or another cause for your cough. Seek medical advice if you are unsure or if you have a cough which has lasted more than three weeks. Most coughs caused by a URTI have cleared up after three weeks.
When you have a cough caused by a URTI, it may be described as being either a chesty cough or a dry cough. If you have a chesty cough this usually means that your lungs are producing more phlegm or mucus than normal, because you have an infection, and you are coughing up extra ‘gunk’. If you have a dry cough this usually means that you are coughing a lot but nothing comes out when you cough.
You May Like: How To Prevent Asthma Attacks
Medical History And Physical Exam
Your doctor will ask about your risk factors for asthma and your symptoms. They may ask also about any known allergies. This includes how often symptoms occur, what seems to trigger your symptoms, when or where symptoms occur, and if your symptoms wake you up at night.
During the physical exam, your doctor may:
- Listen to your breathing and look for symptoms of asthma
- Look for allergic skin conditions, such as eczema
Why Arent Antibiotics Recommended
Antibiotics are drugs that kill or prevent the growth of . Acute is usually caused by viruses, though, so wont help.
Many studies have shown that hardly affect the course of the illness. In the studies, antibiotics reduced the duration of the cough by half a day on average. But they also caused side effects such as diarrhea, nausea or a skin rash in about 3 out of 100 people.
The frequent use of to treat respiratory infections can also lead to the development of resistant . That can result in some medications no longer being effective against certain bacteria. So antibiotics arent recommended for the treatment of acute .
Some people have a higher risk of acute leading to more serious complications , for instance due to a weak immune system, a severe lung or heart condition, or old age. Treatment with may then be a good idea, in order to prevent complications.
Don’t Miss: What To Do When You Have Asthma And No Inhaler
What Are Additional Measures In The Management Of Asthma
What Does My Test Result Mean
For both the PCR and the lateral flow tests, your result will be either:
- negative
Negative
This means that the test did not find coronavirus.
You usually dont need to continue self-isolating if you get a negative result.;But, unless you have had both your vaccinations, you;need to self-isolate if:
- someone you live with tests positive
- youve been told youve been in contact with someone who tested positive.
If you still feel unwell after a negative result, stay at home until youre feeling better. Contact a GP if your symptoms get worse or do not go away.
If you’re being sick, have diarrhoea, or have a high temperature, stay at home until 48 hours after they’ve stopped.
You should check with your employer before going back into work.
You can read more about what your test result means and what to do on the NHS website.
Positive
This means the test found signs of coronavirus.
What you need to do depends on the type of test you had:
Positive PCR test
Positive rapid lateral flow test
If you did a rapid lateral flow test at home and the result was positive, you should self-isolate immediately. You need to report the result and get a PCR test done to confirm the result. You should continue to self-isolate until you get the result of the PCR test, and then follow the advice given when you get the result.;Anyone you live with who has not had both jabs should also self-isolate until you get the result of the PCR test.;
Unclear or void
You May Like: Does Asthma Attack Cause Fever
Should I Be Extra Cautious About Coronavirus If I Have Asthma
Yes. The CDC has released new guidelines for people with asthma, which include the following:
- Stock up on supplies in case you need to self-isolate .
- Stay at home and practice social distancing from those you do not live with .
- Avoid people who are sick, and wash your hands often.
- Avoid crowds.;
- Avoid non-essential travel.
- Clean and disinfect your home and car regularly, especially items you touch often like doorknobs, light switches, cell phones, keyboards, faucets, car door handles, and steering wheels.
- If someone in your home is sick, stay away from them.;
- Avoid sharing personal household items such as cups and towels.
The best way to protect yourself is to keep on top of your asthma and asthma symptoms. Follow these simple asthma management steps:
What Do Cough Suppressants Do
Cough suppressants dont act upon the inflamed mucous membranes in the . Instead, they aim to suppress the urge to cough, so they are rarely used in the treatment of acute . Typical examples of suppressants include codeine and dextromethorphan.
Cough suppressants should only be used in the treatment of severe dry coughs, for a maximum period of two weeks. They shouldnt be used in the treatment of productive coughs: If the urge to cough is suppressed, the phlegm wont be coughed up and out of the lungs.
Besides, there haven’t been any studies on the benefits and drawbacks of cough suppressants in the treatment of acute . The few studies so far have only looked into their effects in simple colds, throat infections and sinusitis. These studies showed the following:
- Codeine doesnt help in the treatment of acute chest colds in adults, children or teenagers. Children under the age of twelve generally shouldnt be prescribed codeine or medications that contain codeine. The same is true for breastfeeding mothers.
- Dextromethorphan can somewhat soothe coughs associated with upper respiratory tract infections in adults only, at least for a short while after it is taken. People with lung conditions like or shouldnt take dextromethorphan. The possible side effects include dizziness and gastrointestinal problems.
Codeine has to be prescribed by a doctor, whereas medications containing dextromethorphan are also available from pharmacies without a prescription.
Read Also: Can Asthma Make You Cough
How To Exercise With Asthma:
1. Keep your blue rescue inhaler on you at all times.2. Check that your asthma is under control. If it’s not under control, exercise could be dangerous.3. Take your medications as directed. If you’re having trouble breathing, you should take your rescue medicine . ;Your doctor may also ask you to take your blue rescue inhaler or another bronchodilator fifteen minutes before you exercise.4. Warm up and cool down properly
- Before exercising, warm up slowly by walking, stretching, and doing other low-level activities.
- After you’ve finished exercising, cool down slowly for at least 10 minutes. Don’t stop exercising all of a sudden. If you’ve been running, taper the run to a walking pace. If you’ve been swimming, finish your swim with a slow paddle. Give your body time to adjust.
5. Protect yourself from other asthma triggers while you’re exercising
;6. If you have symptoms, stop exercising and take your blue rescue inhaler
- Sit up. Wait a few minutes to see if your symptoms improve.
- If your symptoms improve a lot, warm up again and slowly go back to exercising.
- If your symptoms don’t improve, take another dose of your blue rescue inhaler. Wait a few minutes to see if your symptoms improve.
7. If your symptoms still don’t improve, follow these instructions:
- STOP any activity
- Take your blue rescue inhaler
- Sit up
- If the medicine is not working, call 911
- If symptoms are not getting better, keep taking your blue rescue inhaler until the ambulance arrives
How Does Exercise Trigger Asthma Symptoms
Doctors think they know why some people’s asthma is made worse by exercise .Normally, people breathe through their nose. Your nose acts as an air filter. It controls the temperature and humidity of the air before it reaches your lungs.When you exercise, your body wants more air. ;Your breathing speeds up to get more air. You start breathing through your mouth, so you can gulp down more air. But air that comes through your mouth has not been filtered, warmed, or humidified by your nose. This means the air that gets to your airways is cooler and drier than usual.If you have asthma, your extra-sensitive airways don’t like cool dry air. Your airways react: the muscles around the airways twitch and squeeze tighter. Tighter airways mean there is less space for the air to pass through. This makes you wheeze, cough, and feel short of breath.
You May Like: Is Asthma A Type Of Copd
Tips For Wearing A Face Mask With Asthma
The Public Health Agency of Canada currently recommends that Canadians wear non-medical face masks while in public spaces where physical distancing cannot be maintained such as on public transit, or at the grocery store.
Be sure to check your provincial or territorial authority for up-to-date guidance.
Wearing a face mask is NOT a substitute for physical distancing or frequent handwashing. Wearing a non-medical face mask is an extra measure that can be taken to protect those around you. When worn properly, a person wearing a non-medical mask can reduce the spread of their own infectious respiratory droplets.
Make sure you wear your mask properly. It should cover both your nose and mouth. If your mask gets soiled or wet, be sure to wash and dry it before wearing it again. You can read information about appropriate use of non-medical masks, and how to properly place, remove and clean a non-medical mask from the Public Health Agency of Canada.
The vast majority of people with asthma can wear a non-medical mask safely. If you are unable to wear a non-medical mask without experiencing breathing issues, do not wear a mask. Instead, make sure you are practicing physical distancing by maintaining a 2-metre distance. Schedule an appointment with your healthcare provider as soon as possible to go over your Asthma Action Plan and review your asthma symptoms and control. Your healthcare provider may suggest or ask you to consider other options to protect yourself.
/13can Medications Alter Covid Vaccine Response Is There A Need To Switch Medications

COVID vaccines work to generate a robust immune response upon injection. The potential effectiveness of the vaccines may come down to how well your body responds to it.
For the ones suffering from comorbidities, a slow immune response may be a possibility, in some extreme cases. Usage of some drugs may also make the body ‘busy’, leading to a delayed immune response to the vaccine.
That being said, if you are someone enlisted to get the vaccine in the coming while, there are certain medicines and therapies which may make you want to double-check with the doctor or postpone an appointment right now.
Also Check: Is Hot Steam Good For Asthma
Adhere To Your Asthma Action Plan
Manage asthma symptoms in toddlers, children, and adults by developing and following an asthma action plan. Having a plan will help you know what to do in the event of asthma exacerbation symptoms.
- Peak flow numbers indicated which medicines to take and when. Follow the steps as outlined by your plan and your doctor.
- If asthma symptoms get worse, call the doctor who manages your asthma. An asthma action plan should outline what to do in the event of an emergency as well.
Managing Your Asthma During The Pandemic
- Keep taking your controller medication daily or as prescribed. This will help cut your risk of an asthma attack being triggered by any respiratory virus, including COVID-19.
- Carry your reliever inhaler with you every day, in case your asthma symptoms flare up.
- Monitor your asthma symptoms closely and follow your Asthma Action Plan to help you recognize and manage asthma symptoms, and know when to seek advice from your healthcare provider or emergency help.
- If you must travel, pack all asthma medications in your carry-on luggage so it is easily accessible. Pack extra asthma medication in case your travel plans change or are delayed. Be sure to check travel advice and advisories from the;Government of Canadas website.
- Take care of yourself. Get plenty of rest and fluids, and eat good nutritious food.
- Ensure that you speak with your healthcare provider about recommended vaccinations. Getting both the influenza vaccination and pneumococcal disease vaccinationare important steps people with asthma can take to help stay healthy.
- Reach out to Asthma Canadas Asthma & Allergy HelpLinecall-back service to connect with a Certified Respiratory Educator if you have questions about managing your asthma. Call 1-866-787-4050 or email;
Recommended Reading: Is Asthma And Copd The Same Thing
Angiotensin Converting Enzyme Inhibitors
ACE inhibitors are commonly used medicines for the treatment of high blood pressure and heart failure. Common generic-brand forms include lisinopril, ramipril, and many other forms ending in the letters pril. and However, some people have respiratory side effects from this class of medicine, with approximately 10% having a nagging, dry cough. This cough can be mistaken for worsening asthma or other common causes of a cough. Generally, the cough will go away within a few weeks of stopping the ACE inhibitor. However, if a cough is severe, or the ACE inhibitor cannot be stopped, inhaled cromolyn or nedocromil may be useful to treat an ACE inhibitor-induced cough.
What Is An Asthma Attack
An asthma attack may include coughing, chest tightness, wheezing, and trouble breathing. The attack happens in your bodys airways, which are the paths that carry air to your lungs. As the air moves through your lungs, the airways become smaller, like the branches of a tree are smaller than the tree trunk. During an asthma attack, the sides of the airways in your lungs swell and the airways shrink. Less air gets in and out of your lungs, and mucous that your body makes clogs up the airways.
You can control your asthma by knowing the warning signs of an asthma attack, staying away from things that cause an attack, and following your doctors advice. When you control your asthma:
- you wont have symptoms such as wheezing or coughing,
- youll sleep better,
- you wont miss work or school,
- you can take part in all physical activities, and
- you wont have to go to the hospital.
Also Check: What Is Asthma Characterized By
